Journal of Peking University (Health Sciences) ›› 2026, Vol. 58 ›› Issue (2): 359-364. doi: 10.19723/j.issn.1671-167X.2026.02.021
Previous Articles Next Articles
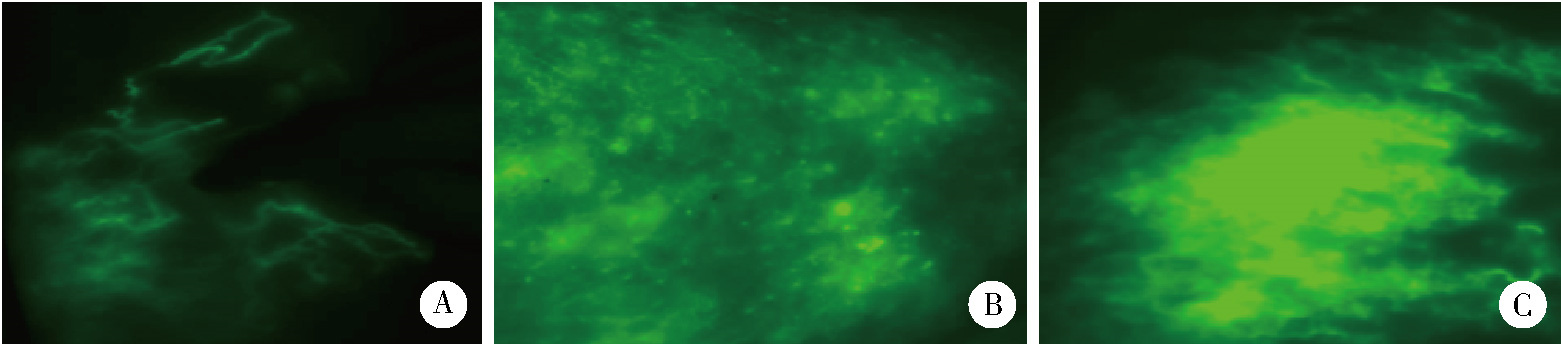
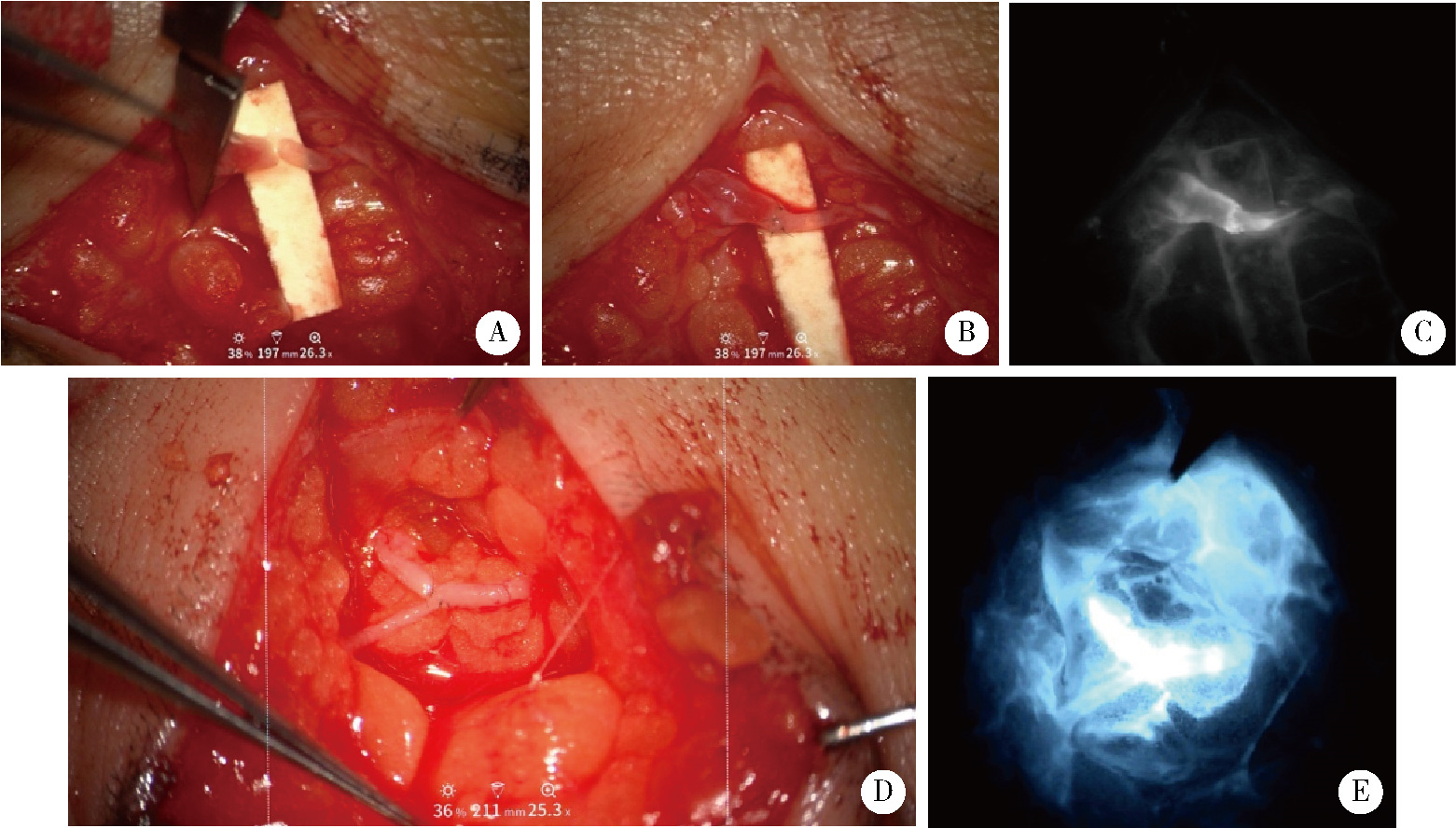
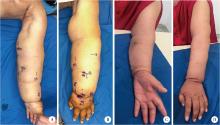
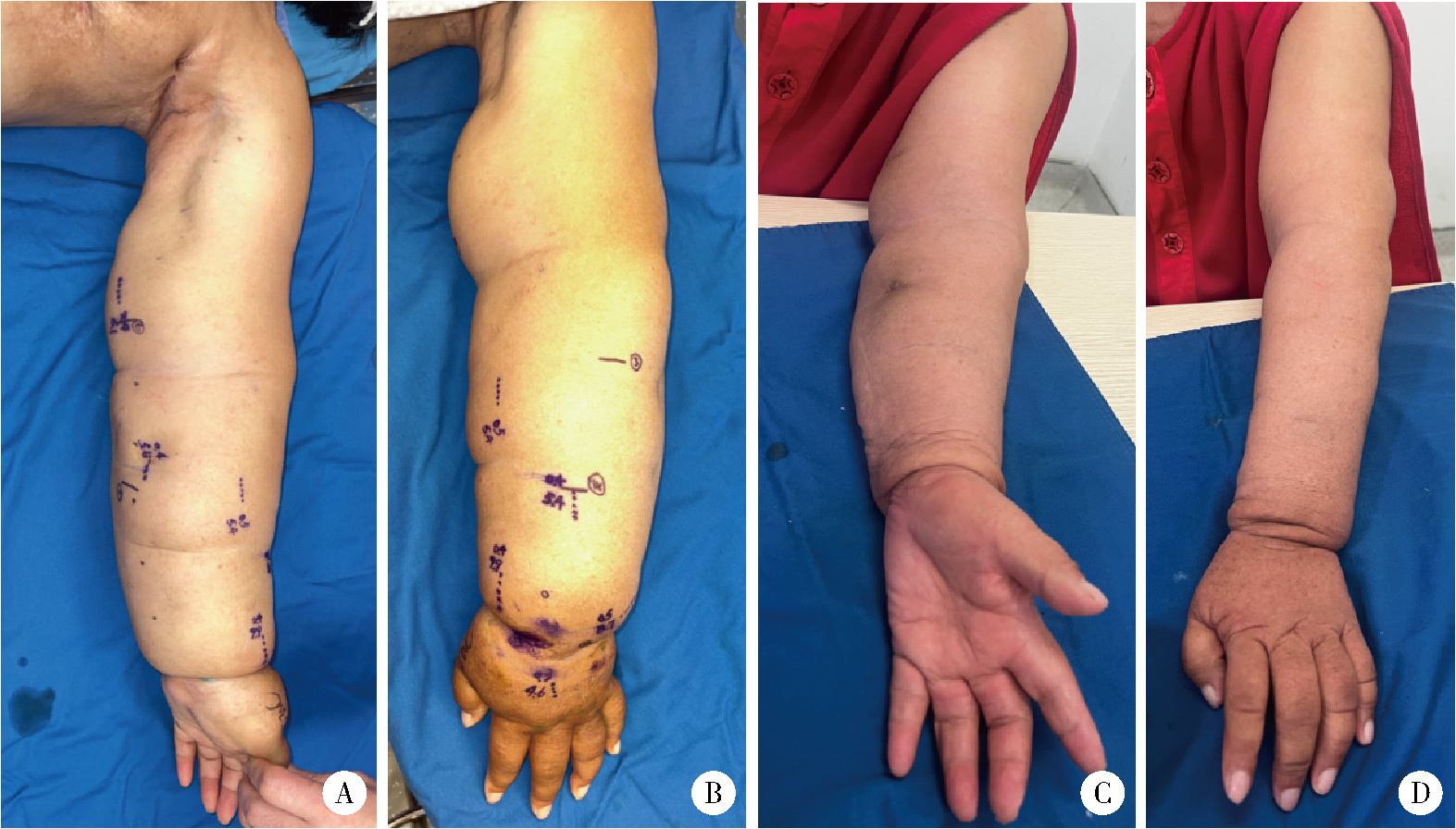
Super microsurgical lymphaticovenular anastomosis for limb lymphedema: An outcome analysis based on clinical stage and indocyanine green pattern
Jingheng WU1,*( ), Yunhao XUE1, Shanlin CHEN1, Yintao GUO2, Yuntao LIU2, Wei ZHANG2
), Yunhao XUE1, Shanlin CHEN1, Yintao GUO2, Yuntao LIU2, Wei ZHANG2
- 1. Department of Hand Surgery, Beijing Jishuitan Hospital, Capital Medical University, Beijing 100035, China
2. Department of Hand and Microsurgery, Zhengzhou Central Hospital Affiliated to Zhengzhou University, Zhengzhou 450007, China
CLC Number:
- R622.4
| 1 |
Cheville AL, McLaughlin SA, Glaser GE, et al. Cancer related lymphedema[J/OL]. BMJ, 2025, 390(2025-07-03)[2025-09-10]. https://pubmed.ncbi.nlm.nih.gov/41065270.
|
| 2 |
doi: 10.1002/micr.22115 |
| 3 |
doi: 10.1097/PRS.0000000000009247 |
| 4 |
doi: 10.1055/a-2530-5875 |
| 5 |
doi: 10.1007/s12032-024-02421-6 |
| 6 |
doi: 10.1080/17434440.2024.2419476 |
| 7 |
doi: 10.1055/s-2003-40575 |
| 8 |
doi: 10.1002/micr.1025 |
| 9 |
doi: 10.1016/j.bjps.2012.05.026 |
| 10 |
doi: 10.1055/s-0032-1311691 |
| 11 |
doi: 10.1097/01.sap.0000120319.89926.07 |
| 12 |
doi: 10.1097/PRS.0b013e3182268da8 |
| 13 |
doi: 10.1097/PRS.0b013e31820cf5c6 |
| 14 |
doi: 10.1002/micr.20980 |
| 15 |
doi: 10.1002/bjs.9588 |
|
||