Journal of Peking University (Health Sciences) ›› 2026, Vol. 58 ›› Issue (2): 351-358. doi: 10.19723/j.issn.1671-167X.2026.02.020
Previous Articles Next Articles
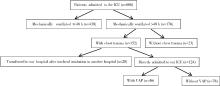
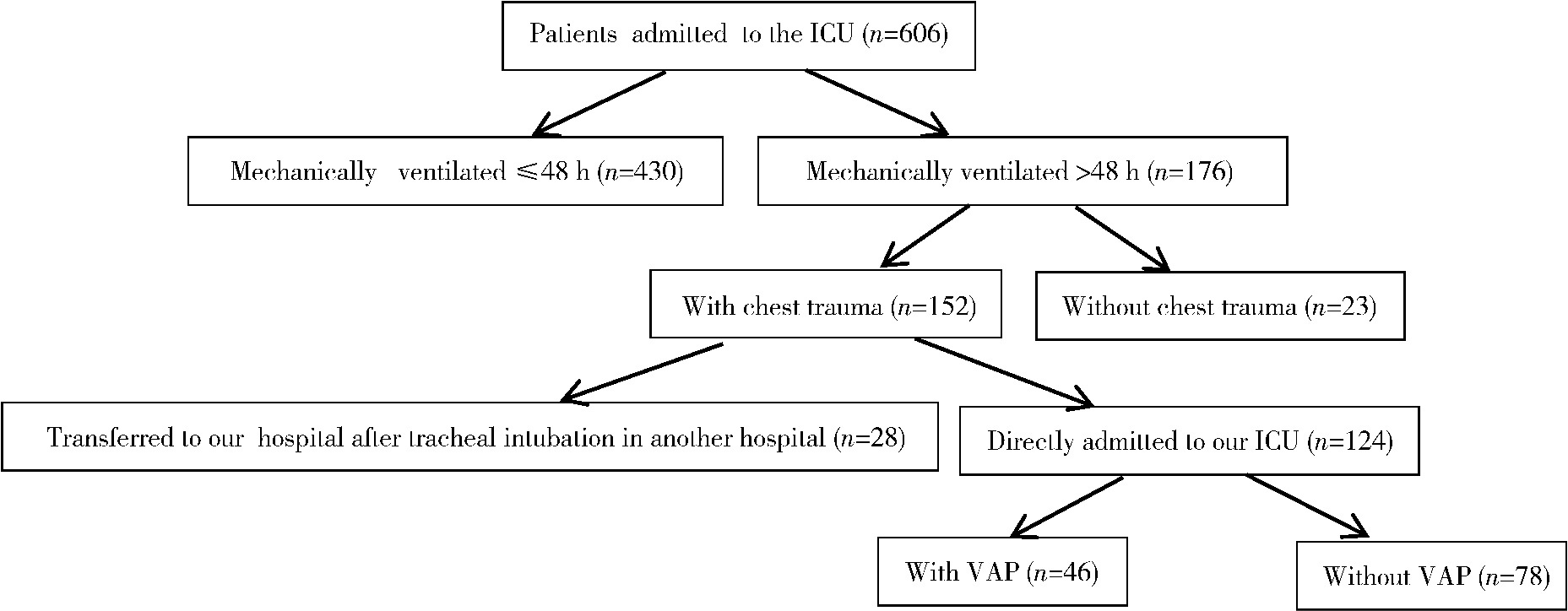
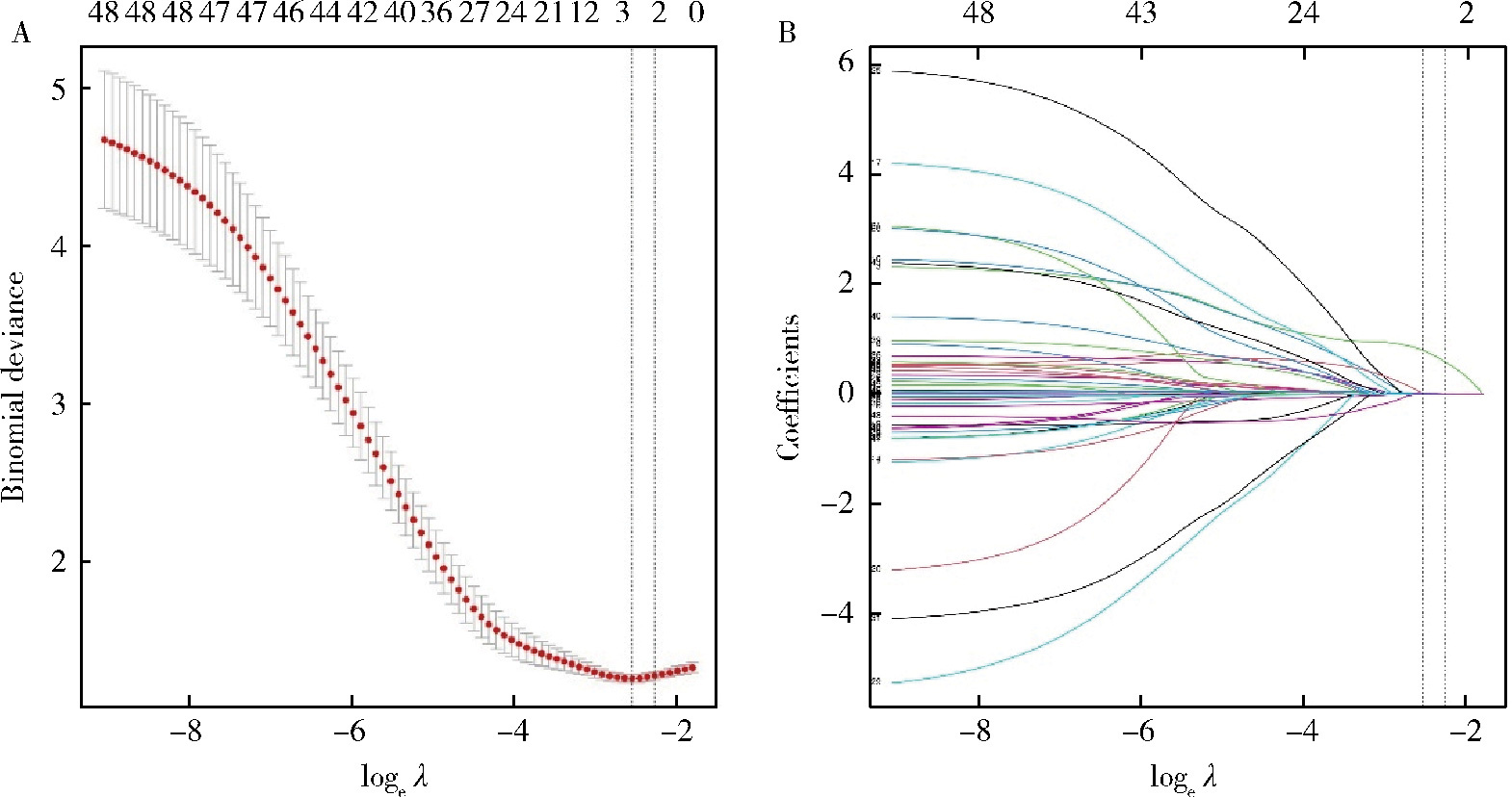
Risk factors for ventilator-associated pneumonia in patients with chest trauma in intensive care unit
Jie ZHAO, Chun FU, Xiujuan ZHAO, Haiyan XUE, Shu LI, Zhenzhou WANG, Fengxue ZHU*( )
)
- Department of Critical Care Medicine, Trauma Treatment Center, Peking University People's Hospital, Beijing 100044, China
CLC Number:
- R563.1
| 1 |
中华医学会呼吸病学分会感染学组. 中国成人医院获得性肺炎与呼吸机相关性肺炎诊断和治疗指南(2018年版)[J]. 中华结核和呼吸杂志, 2018, 41 (4): 255- 280.
|
| 2 |
doi: 10.1093/cid/ciy543 |
| 3 |
doi: 10.1016/j.jcrc.2023.154284 |
| 4 |
doi: 10.1007/s00134-020-05980-0 |
| 5 |
doi: 10.3390/antibiotics9020051 |
| 6 |
doi: 10.1186/cc13775 |
| 7 |
doi: 10.1093/cid/cis926 |
| 8 |
doi: 10.4187/respcare.05500742 |
| 9 |
doi: 10.1016/j.ijid.2013.02.004 |
| 10 |
doi: 10.4103/0972-5229.130570 |
| 11 |
doi: 10.4066/AMJ.2013.1710 |
| 12 |
|
| 13 |
|
| 14 |
doi: 10.1007/s00268-019-05286-3 |
| 15 |
doi: 10.5455/jmas.42509 |
| 16 |
|
| 17 |
doi: 10.1007/s00134-004-2514-z |
| 18 |
doi: 10.1016/j.ijid.2015.07.005 |
| 19 |
doi: 10.1016/j.amjsurg.2015.06.029 |
| 20 |
doi: 10.5090/kjtcs.2017.50.5.346 |
| 21 |
doi: 10.5847/wjem.j.1920-8642.2018.03.007 |
| 22 |
doi: 10.1089/sur.2006.069 |
| 23 |
doi: 10.1016/j.chest.2020.06.064 |
| 24 |
doi: 10.1007/s12028-019-00773-w |
| 25 |
doi: 10.1016/j.joms.2015.08.018 |
| 26 |
doi: 10.3390/jcm10153319 |
| 27 |
doi: 10.1016/j.jocn.2023.06.004 |
| 28 |
|
| 29 |
doi: 10.3390/jpm12040597 |
| 30 |
doi: 10.1186/s12879-017-2566-7 |
| 31 |
doi: 10.4103/0974-2700.120364 |
| 32 |
doi: 10.5005/jp-journals-10071-24465 |
| 33 |
|
| [1] | Hui WEI, Jingfeng ZHANG, Zhongqiang YAO, Jinxia ZHAO. Clinical characteristics and relevant factors of rheumatoid arthritis patients with anemia of chronic disease [J]. Journal of Peking University (Health Sciences), 2026, 58(2): 307-312. |
| [2] | Bowen LI, Qiang ZHANG, Yixin SUN. Establishment and validation of a risk prediction model for scoliosis after Nuss procedure in children and young adults with pectus excavatum [J]. Journal of Peking University (Health Sciences), 2025, 57(5): 941-946. |
| [3] | Xiaoyong YANG, Fan ZHANG, Lulin MA, Cheng LIU. Clinical characteristics and influencing factors of extraglandular invasion of prostatic ductal adenocarcinoma [J]. Journal of Peking University (Health Sciences), 2025, 57(5): 956-960. |
| [4] | Wei LIU, Wen GUO, Zhe GUO, Chunyan LI, Yunlong LI, Siqi LIU, Liang ZHANG, Hui SONG. Risk factors associated with non-radiographic bone erosion in patients with gout [J]. Journal of Peking University (Health Sciences), 2025, 57(4): 735-739. |
| [5] | Mengxi LU, Qiuping LIU, Tianjing ZHOU, Xiaofei LIU, Yexiang SUN, Peng SHEN, Hongbo LIN, Xun TANG, Pei GAO. Association of triglyceride-glucose index and cardiovascular disease in a community-based Chinese cohort [J]. Journal of Peking University (Health Sciences), 2025, 57(3): 430-435. |
| [6] | Huaqiu GUO, Zhe WANG, Xue YANG, Jie BAI. Clinical features and risk factors of patients with oral bleeding in dental emergency [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 142-147. |
| [7] | Minting DENG, Nan WANG, Bin XIA, Yuming ZHAO, Junxia ZHU. Factors associated with spontaneous re-eruption of traumatically intruded permanent anterior teeth in children and adolescents [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 148-153. |
| [8] | Yukai LI, Hongyan WANG, Liang LUO, Yun LI, Chun LI. Clinical significance of antiphospholipid antibodies in Behcet disease with thrombosis [J]. Journal of Peking University (Health Sciences), 2024, 56(6): 1036-1040. |
| [9] | Yang TIAN, Yongzheng HAN, Jiao LI, Mingya WANG, Yinyin QU, Jingchao FANG, Hui JIN, Min LI, Jun WANG, Mao XU, Shenglin WANG, Xiangyang GUO. Incidence and risk factors of postoperative epidural hematoma following anterior cervical spine surgery [J]. Journal of Peking University (Health Sciences), 2024, 56(6): 1058-1064. |
| [10] | Mingrui WANG, Jinhui LAI, Jiaxiang JI, Xinwei TANG, Haopu HU, Qi WANG, Kexin XU, Tao XU, Hao HU. Risk factors for decreased quality of life in patients with kidney stones predicted by the Chinese version of Wisconsin stone quality of life questionnaire [J]. Journal of Peking University (Health Sciences), 2024, 56(6): 1069-1074. |
| [11] | Zhicun LI, Tianyu WU, Lei LIANG, Yu FAN, Yisen MENG, Qian ZHANG. Risk factors analysis and nomogram model construction of postoperative pathological upgrade of prostate cancer patients with single core positive biopsy [J]. Journal of Peking University (Health Sciences), 2024, 56(5): 896-901. |
| [12] | Ye YAN,Xiaolong LI,Haizhui XIA,Xuehua ZHU,Yuting ZHANG,Fan ZHANG,Ke LIU,Cheng LIU,Lulin MA. Analysis of risk factors for long-term overactive bladder after radical prostatectomy [J]. Journal of Peking University (Health Sciences), 2024, 56(4): 589-593. |
| [13] | Yan CHEN,Kuangmeng LI,Kai HONG,Shudong ZHANG,Jianxing CHENG,Zhongjie ZHENG,Wenhao TANG,Lianming ZHAO,Haitao ZHANG,Hui JIANG,Haocheng LIN. Retrospective study on the impact of penile corpus cavernosum injection test on penile vascular function [J]. Journal of Peking University (Health Sciences), 2024, 56(4): 680-686. |
| [14] | Bo PANG,Tongjun GUO,Xi CHEN,Huaqi GUO,Jiazhang SHI,Juan CHEN,Xinmei WANG,Yaoyan LI,Anqi SHAN,Hengyi YU,Jing HUANG,Naijun TANG,Yan WANG,Xinbiao GUO,Guoxing LI,Shaowei WU. Personal nitrogen oxides exposure levels and related influencing factors in adults over 35 years old in Tianjin and Shanghai [J]. Journal of Peking University (Health Sciences), 2024, 56(4): 700-707. |
| [15] | Jing HE,Zhongze FANG,Ying YANG,Jing LIU,Wenyao MA,Yong HUO,Wei GAO,Yangfeng WU,Gaoqiang XIE. Relationship between lipid metabolism molecules in plasma and carotid atheroscle-rotic plaques, traditional cardiovascular risk factors, and dietary factors [J]. Journal of Peking University (Health Sciences), 2024, 56(4): 722-728. |
|
||