Journal of Peking University (Health Sciences) ›› 2020, Vol. 52 ›› Issue (2): 269-274. doi: 10.19723/j.issn.1671-167X.2020.02.012
Previous Articles Next Articles
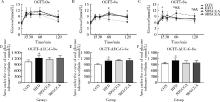
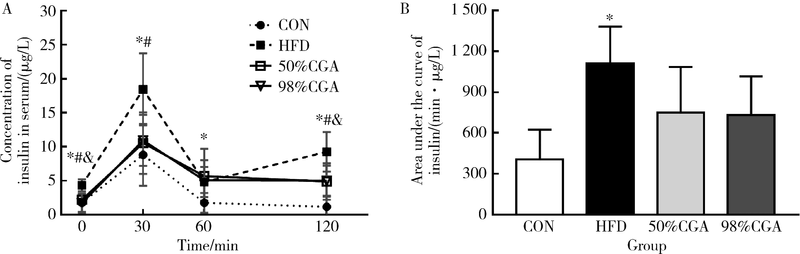
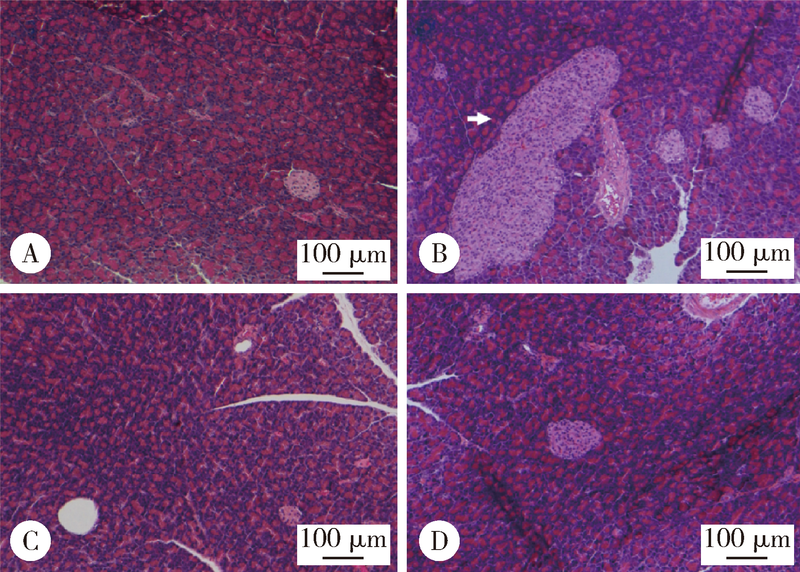
Effects of chlorogenic acid on glucose tolerance and its curve characteristics in high-fat diet-induced obesity rats
Cheng-cheng GUO,Xiao-yuan ZHANG,Ying-xiang YU,Lan XIE,Cui-qing CHANG( )
)
- Institute of Sports Medicine, Peking University Third Hospital, Beijing 100191, China
CLC Number:
- R587.1
| [1] | Wang L, Gao P, Zhang M , et al. Prevalence and ethnic pattern of diabetes and prediabetes in China in 2013[J]. JAMA, 2017,317(24):2515-2523. |
| [2] | Li G, Zhang P, Wang J , et al. Cardiovascular mortality, all-cause mortality, and diabetes incidence after lifestyle intervention for people with impaired glucose tolerance in the da qing diabetes prevention study: a 23-year follow-up study[J]. Lancet Diabetes Endocrinol, 2014,2(6):474-480. |
| [3] | Unwin N, Shaw J, Zimmet P , et al. Impaired glucose tolerance and impaired fasting glycaemia: the current status on definition and intervention[J]. Diabet Med, 2002,19(9):708-723. |
| [4] | Hulman A, Witte DR, Vistisen D , et al. Pathophysiological characteristics underlying different glucose response curves: a latent class trajectory analysis from the prospective EGIR-RISC study[J]. Diabetes Care, 2018,41(8):1740-1748. |
| [5] | Tura A, Morbiducci U, Sbrignadello S , et al. Shape of glucose, insulin, C-peptide curves during a 3-h oral glucose tolerance test: any relationship with the degree of glucose tolerance[J]. Am J Physiol Regul Integr Comp Physiol, 2011,300(4):R941-R948. |
| [6] | Abdul-Ghani MA, Williams K, Defronzo R , et al. Risk of progression to type 2 diabetes based on relationship between postload plasma glucose and fasting plasma glucose[J]. Diabetes Care, 2006,29(7):1613-1618. |
| [7] | Hayashi T, Boyko EJ, Sato KK , et al. Patterns of insulin concentration during the OGTT predict the risk of type 2 diabetes in Japanese Americans[J]. Diabetes Care, 2013,36(5):1229-1235. |
| [8] | Kramer CK, Vuksan V, Choi H , et al. Emerging parameters of the insulin and glucose response on the oral glucose tolerance test: reproducibility and implications for glucose homeostasis in individuals with and without diabetes[J]. Diabetes Res Clin Pract, 2014,105(1):88-95. |
| [9] | Wang X, Zhao X, Zhou R , et al. Delay in glucose peak time during the oral glucose tolerance test as an indicator of insulin resistance and insulin secretion in type 2 diabetes patients[J]. J Diabetes Investig, 2018,9(6):1288-1295. |
| [10] | Kramer CK, Ye C, Hanley AJ , et al. Delayed timing of post-challenge peak blood glucose predicts declining beta cell function and worsening glucose tolerance over time: insight from the first year postpartum[J]. Diabetologia, 2015,58(6):1354-1362. |
| [11] | Kanauchi M, Kimura K, Kanauchi K , et al. Beta-cell function and insulin sensitivity contribute to the shape of plasma glucose curve during an oral glucose tolerance test in non-diabetic individuals[J]. Int J Clin Pract, 2005,59(4):427-432. |
| [12] | Chung ST, Ha J, Onuzuruike AU , et al. Time to glucose peak during an oral glucose tolerance test identifies prediabetes risk[J]. Clin Endocrinol (Oxf), 2017,87(5):484-491. |
| [13] | Li G, Zhang P, Wang J , et al. The long-term effect of lifestyle interventions to prevent diabetes in the China da qing diabetes prevention study: a 20-year follow-up study[J]. Lancet, 2008,371(9626):1783-1789. |
| [14] | Zuniga LY , Aceves-de LMM, Gonzalez-Ortiz M, et al. Effect of chlorogenic acid administration on glycemic control, insulin secretion, and insulin sensitivity in patients with impaired glucose tolerance[J]. J Med Food, 2018,21(5):469-473. |
| [15] | Ma Y, Gao M, Liu D . Chlorogenic acid improves high fat diet-induced hepatic steatosis and insulin resistance in mice[J]. Pharm Res, 2015,32(4):1200-1209. |
| [16] | Jin S, Chang C, Zhang L , et al. Chlorogenic acid improves late diabetes through adiponectin receptor signaling pathways in db/db mice[J]. PLoS One, 2015,10(4):e120842. |
| [17] | Panchal SK, Poudyal H, Waanders J , et al. Coffee extract attenuates changes in cardiovascular and hepatic structure and function without decreasing obesity in high-carbohydrate, high-fat diet-fed male rats[J]. J Nutr, 2012,142(4):690-697. |
| [18] | Hariri N, Thibault L . High-fat diet-induced obesity in animal models[J]. Nutr Res Rev, 2010,23(2):270-299. |
| [19] | Le Floch JP, Escuyer P, Baudin E , et al. Blood glucose area under the curve. Methodological aspects[J]. Diabetes Care, 1990,13(2):172-175. |
| [20] | Tschritter O, Fritsche A, Shirkavand F , et al. Assessing the shape of the glucose curve during an oral glucose tolerance test[J]. Diabetes Care, 2003,26(4):1026-1033. |
| [21] | Wong SK, Chin KY, Suhaimi FH , et al. The effects of a modified high-carbohydrate high-fat diet on metabolic syndrome parameters in male rats[J]. Exp Clin Endocrinol Diabetes, 2018,126(4):205-212. |
| [22] | Joung KH, Ju SH, Kim JM , et al. Clinical implications of using post-challenge plasma glucose levels for early diagnosis of type 2 diabetes mellitus in older individuals[J]. Diabetes Metab J, 2018,42(2):147-154. |
| [1] | Yihang ZHANG, Shan CAI, Ziyue CHEN, Yunfei LIU, Jiajia DANG, Di SHI, Jiaxin LI, Tianyu HUANG, Yi SONG. Establishment of outcome indicators for the implementation of comprehensive intervention for multimorbidity of myopia and obesity among children and adolescents based on the RE-AIM framework [J]. Journal of Peking University (Health Sciences), 2025, 57(3): 436-441. |
| [2] | Shunkai LIU, Weihua CAO, Jun LV, Canqing YU, Tao HUANG, Dianjianyi SUN, Chunxiao LIAO, Yuanjie PANG, Runhua HU, Ruqin GAO, Min YU, Jinyi ZHOU, Xianping WU, Yu LIU, Wenjing GAO, Liming LI. Association between DNA methylation clock and obesity-related indicators: A longitudinal twin study [J]. Journal of Peking University (Health Sciences), 2025, 57(3): 456-464. |
| [3] | Ping LI, Haixue WANG, Xiao GAO, Yajing HAN, Hui WANG, Haijun WANG, Yingying MU. A randomized controlled trial of weight management based on mobile health techno-logy among overweight or obese pregnant women [J]. Journal of Peking University (Health Sciences), 2025, 57(3): 465-472. |
| [4] | Huili LIU, Bei WEN, Xue BAI, Ming'an CHEN, Min LI. Association between weight-adjusted waist index and pain: A cross-sectional study [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 178-184. |
| [5] | Jing CHEN,Rui SHAN,Wucai XIAO,Xiaorui ZHANG,Zheng LIU. Association between self-control and co-occurrence of depressive symptoms and overweight or obesity during adolescence and early adulthood: A ten-year prospective cohort study based on national surveys [J]. Journal of Peking University (Health Sciences), 2024, 56(3): 397-402. |
| [6] | Chu-yun CHEN,Peng-fei SUN,Jing ZHAO,Jia JIA,Fang-fang FAN,Chun-yan WANG,Jian-ping LI,Yi-meng JIANG,Yong HUO,Yan ZHANG. Related factors of endogenous erythropoietin and its association with 10-year risks of cardiovascular disease in a community-based Chinese study [J]. Journal of Peking University (Health Sciences), 2023, 55(6): 1068-1073. |
| [7] | Jing CHEN,Wu-cai XIAO,Rui SHAN,Jie-yun SONG,Zheng LIU. Influence of rs2587552 polymorphism of DRD2 gene on the effect of a childhood obesity intervention: A prospective, parallel-group controlled trial [J]. Journal of Peking University (Health Sciences), 2023, 55(3): 436-441. |
| [8] | Jia-jia DANG,Shan CAI,Pan-liang ZHONG,Ya-qi WANG,Yun-fei LIU,Di SHI,Zi-yue CHEN,Yi-hang ZHANG,Pei-jin HU,Jing LI,Jun MA,Yi SONG. Association of outdoor artificial light at night exposure with overweight and obesity among children and adolescents aged 9 to 18 years in China [J]. Journal of Peking University (Health Sciences), 2023, 55(3): 421-428. |
| [9] | Tao MA,Yan-hui LI,Man-man CHEN,Ying MA,Di GAO,Li CHEN,Qi MA,Yi ZHANG,Jie-yu LIU,Xin-xin WANG,Yan-hui DONG,Jun MA. Associations between early onset of puberty and obesity types in children: Based on both the cross-sectional study and cohort study [J]. Journal of Peking University (Health Sciences), 2022, 54(5): 961-970. |
| [10] | Xiao-yuan ZHANG,Cheng-cheng GUO,Ying-xiang YU,Lan XIE,Cui-qing CHANG. Establishment of high-fat diet-induced obesity and insulin resistance model in rats [J]. Journal of Peking University (Health Sciences), 2020, 52(3): 557-563. |
| [11] | Xiao-na NA,Zhu ZHU,Yang-yang CHEN,Dong-ping WANG,Hao-jie WANG,Yang SONG,Xiao-chuan MA,Pei-yu WANG,Ai-ping LIU. Associations of distribution of time spent in physical activity and sedentary behavior with obesity [J]. Journal of Peking University (Health Sciences), 2020, 52(3): 486-491. |
| [12] | DONG Yan-hui, SONG Yi, DONG Bin, ZOU Zhi-yong, WANG Zheng-he, YANG Zhao-geng, WANG Xi-jie, LI Yan-hui, MA Jun. Association between the blood pressure status and nutritional status among Chinese students aged 7-18 years in 2014: based on the national blood pressure reference for Chinese children and adolescents [J]. Journal of Peking University(Health Sciences), 2018, 50(3): 422-428. |
| [13] | WU Yu-jia, CHI Xiao-pei, CHEN Feng, DENG Xu-liang. Salivary microbiome in people with obesity: a pilot study [J]. Journal of Peking University(Health Sciences), 2018, 50(1): 5-12. |
| [14] | DU Yi-qing, LIU Hui-xin, LIU Chun-lei, DUN Yao-jun, LI Qing, YU Lu-ping, LIU Shi-jun, CHEN Li-li, WANG Xiao-feng, XU Tao. Analysis of metabolic factors and relevance with the grade and stage in patients with renal cell carcinoma [J]. Journal of Peking University(Health Sciences), 2016, 48(4): 612-617. |
| [15] | CHENG Lan, LI Qin, SONG Yi, MA Jun, WANG Hai-Jun. Association of physical activities, sedentary behaviors with overweight/obesity in 9-11 year-old Chinese primary school students [J]. Journal of Peking University(Health Sciences), 2016, 48(3): 436-441. |
|
||