Journal of Peking University (Health Sciences) ›› 2026, Vol. 58 ›› Issue (2): 365-371. doi: 10.19723/j.issn.1671-167X.2026.02.022
Previous Articles Next Articles
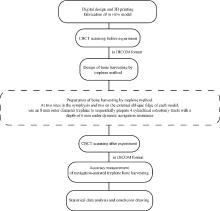
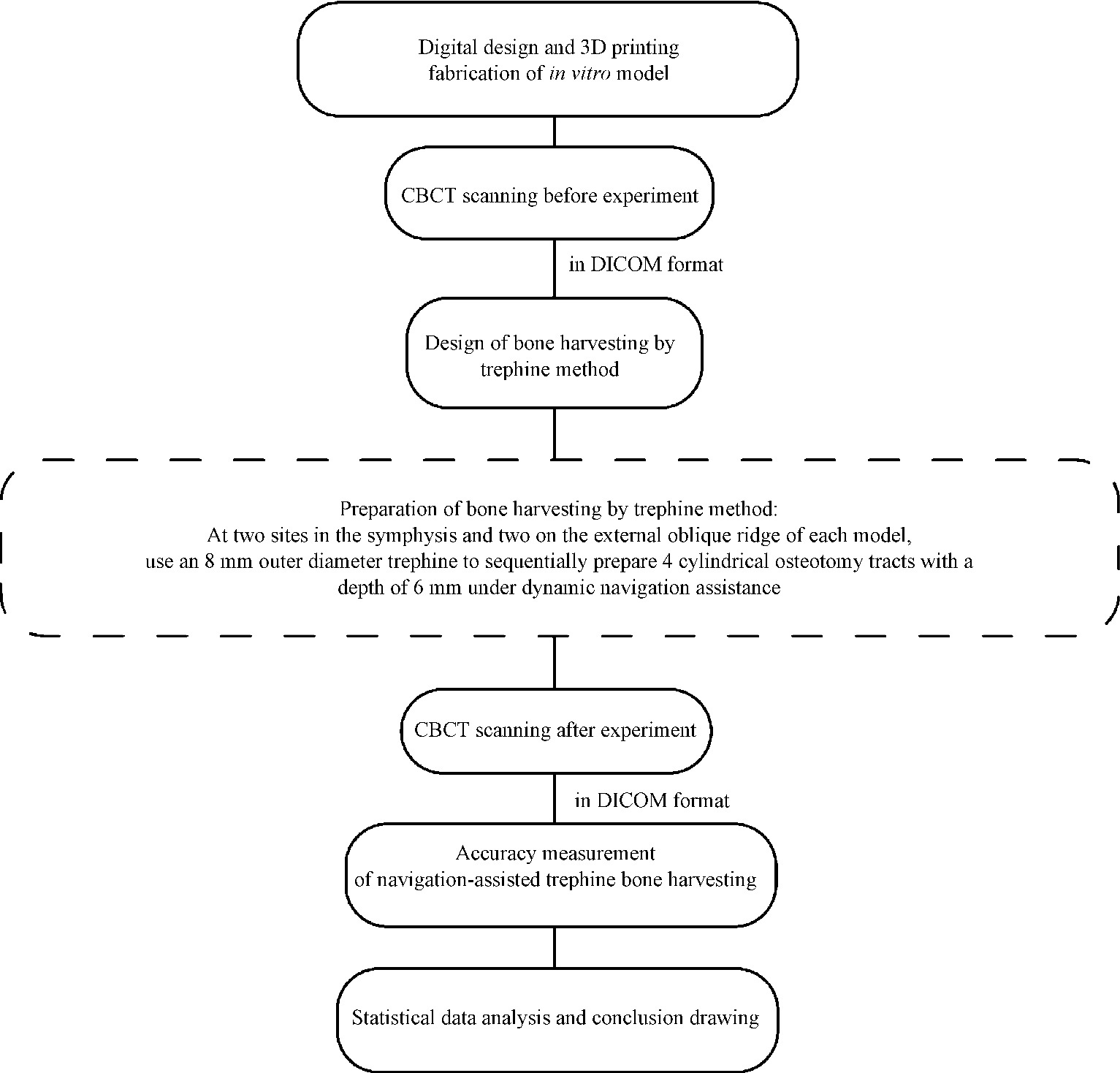
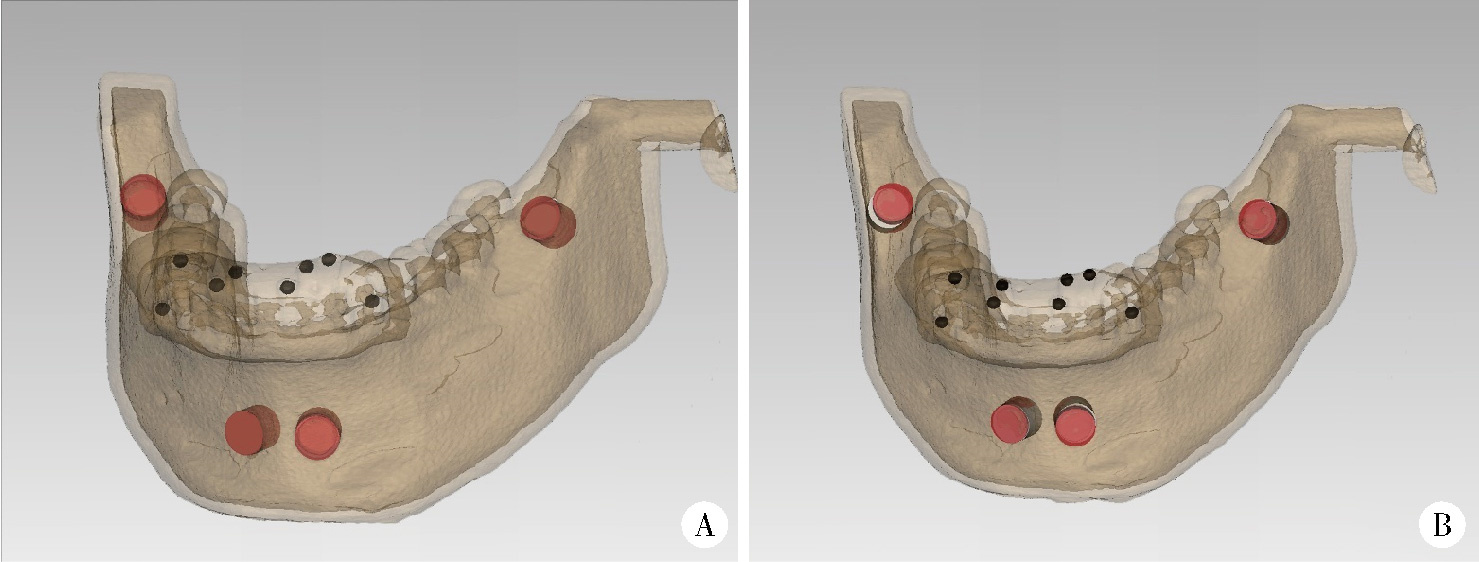
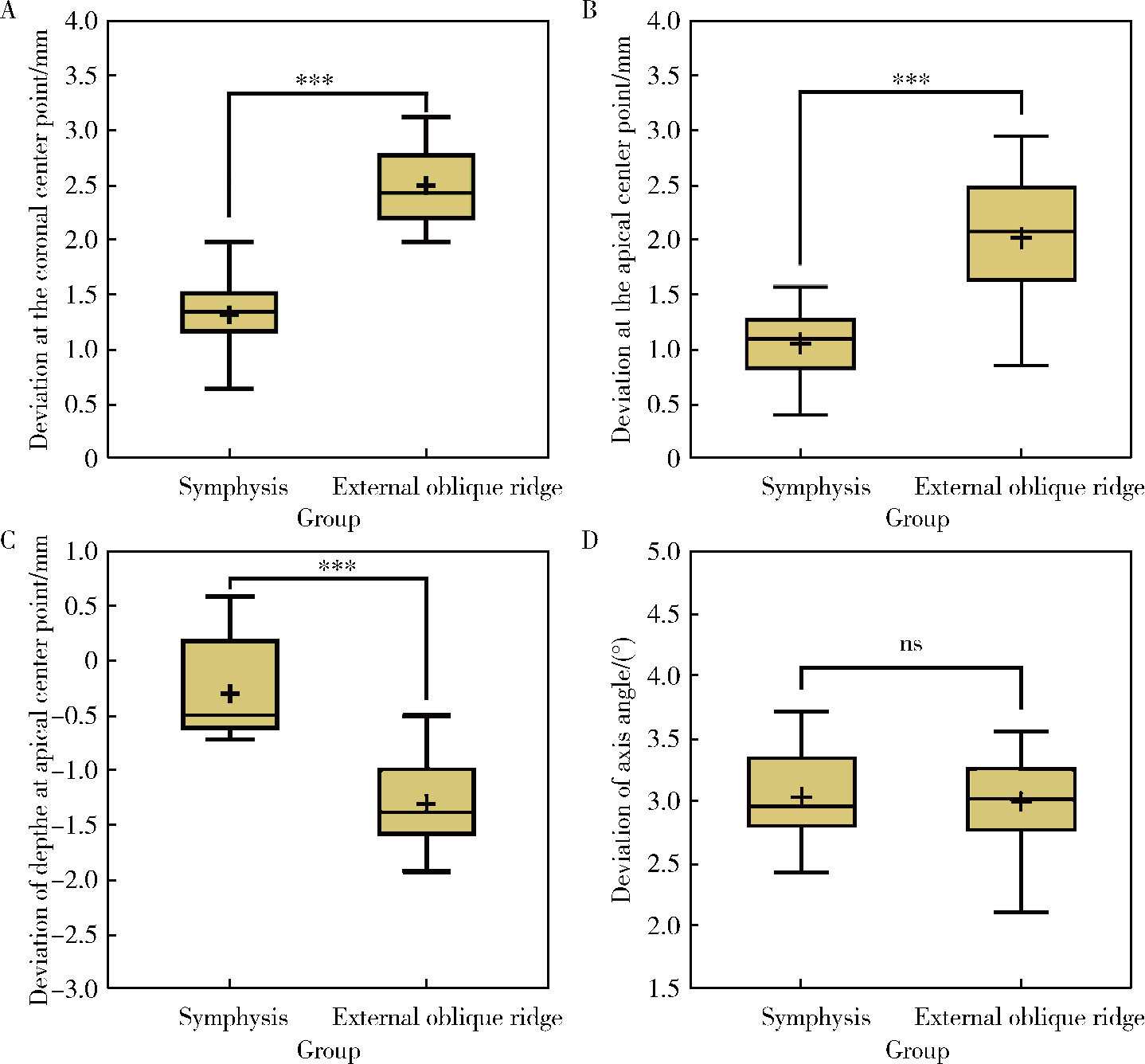
Accuracy of dynamic navigation-assisted trephine method for bone harvesting
Jiayu LIU, Ning ZHU, Yuchen CHANG, Xianming GAO, Yu ZHANG*( )
)
- Department of Oral Implantology, Peking University School and Hospital of Stomatology & National Center for Stomatology & National Clinical Research Center for Oral Diseases & National Engineering Research Center of Oral Biomaterials and Digital Medical Devices & Beijing Key Laboratory of Digital Stomatology, Beijing 100081, China
CLC Number:
- R783
| 1 |
doi: 10.1016/j.injury.2011.03.033 |
| 2 |
doi: 10.1016/j.ijom.2015.11.001 |
| 3 |
doi: 10.11607/jomi.4117 |
| 4 |
doi: 10.1016/j.injury.2020.04.041 |
| 5 |
doi: 10.1097/SCS.0000000000002177 |
| 6 |
doi: 10.11607/jomi.5998 |
| 7 |
doi: 10.1186/1746-160X-9-3 |
| 8 |
|
| 9 |
doi: 10.1111/j.1708-8208.2012.00440.x |
| 10 |
doi: 10.1111/cid.12431 |
| 11 |
doi: 10.1016/j.jcms.2014.01.011 |
| 12 |
|
| 13 |
doi: 10.3390/ma12223802 |
| 14 |
|
| 15 |
doi: 10.1016/j.prosdent.2019.04.014 |
| 16 |
doi: 10.1016/j.prosdent.2021.11.034 |
| 17 |
doi: 10.1016/j.joms.2015.09.022 |
| 18 |
doi: 10.1111/j.1600-0501.2010.02070.x |
| 19 |
doi: 10.1016/j.coms.2019.08.001 |
| 20 |
刘思民, 赵一姣, 王晓燕, 等. 动态导航下不同深度环钻定位精确度的体外评价[J]. 北京大学学报(医学版), 2022, 54 (2): 146- 152.
doi: 10.19723/j.issn.1671-167X.2022.01.023 |
| 21 |
doi: 10.1186/s40729-020-00272-0 |
| 22 |
|
| 23 |
doi: 10.1007/s11517-018-1861-9 |
| 24 |
满毅, 周楠, 杨醒眉. 动态实时导航在口腔种植领域中的临床应用及新进展[J]. 口腔疾病防治, 2020, 28 (6): 341- 348.
|
| 25 |
doi: 10.1111/cid.12958 |
| 26 |
陶宝鑫, 蓝耕良, 黄伟, 等. 动态导航技术辅助无牙颌种植精度分析[J]. 上海交通大学学报(医学版), 2022, 42 (9): 1353- 1360.
|
| 27 |
王磊, 伍颖颖, 满毅. 动态导航技术中植入位点骨质量对种植精度的影响[J]. 口腔颌面外科杂志, 2022, 32 (3): 174- 181.
|
| 28 |
doi: 10.1111/clr.13719 |
| 29 |
doi: 10.1111/clr.13563 |
| 30 |
doi: 10.3390/jcm8122123 |
| 31 |
林后学, 郭松松, 何佳宜, 等. 下颌骨颏部骨皮质增龄性变化的锥形束CT研究[J]. 中国CT和MRI杂志, 2016, 14 (9): 15- 18.
|
| [1] | Yongtao YANG, Yuwen TIAN, Shenyao SHAN, Wenbo LI, Xiangyi SHANG, Yizhen WANG, Shuwei GUO, Zixiang GAO, Aonan WEN, Yijiao ZHAO, Yong WANG. A multi-view stereo vision methodology for digital soft-tissue impressions in fixed implant rehabilitation of edentulous patients [J]. Journal of Peking University (Health Sciences), 2026, 58(1): 126-132. |
| [2] | Yulan WANG, Hao ZENG, Yufeng ZHANG. Current situation and exploration of clinical transformation of plasmatrix in oral implantology [J]. Journal of Peking University (Health Sciences), 2025, 57(5): 836-840. |
| [3] | Ziyang YU, Houzuo GUO, Xi JIANG, Weihua HAN, Ye LIN. Imaging study of osteogenesis in maxillary sinus segment of zygomatic implants [J]. Journal of Peking University (Health Sciences), 2025, 57(5): 967-974. |
| [4] | Fangru LIN, Zhihui TANG. Correlation analysis of peri-implant health after single-tooth dental implant [J]. Journal of Peking University (Health Sciences), 2025, 57(2): 347-353. |
| [5] | Yutong SHI, Yiping WEI, Wenjie HU, Tao XU, Haoyun ZHANG. Evaluation of micro crestal flap-alveolar ridge preservation following extraction of mandibular molars with severe periodontitis [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 33-41. |
| [6] | Junnan NIE, Jiayun DONG, Ruifang LU. Analysis of soft tissue healing after keratinized tissue augmentation in reconstructed jaws [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 57-64. |
| [7] | Juan WANG, Lixin QIU, Huajie YU. Influence of emergence profile designs on the peri-implant tissue in the mandibular molar: A randomized controlled trial [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 65-72. |
| [8] | Hong LI, Feifei MA, Jinlong WENG, Yang DU, Binzhang WU, Feng SUN. Accuracy of dynamic navigation system for immediate dental implant placement [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 85-90. |
| [9] | Han ZHANG,Yixuan QIN,Diyuan WEI,Jie HAN. A preliminary study on compliance of supportive treatment of patients with periodontitis after implant restoration therapy [J]. Journal of Peking University (Health Sciences), 2024, 56(1): 39-44. |
| [10] | Congwei WANG,Min GAO,Yao YU,Wenbo ZHANG,Xin PENG. Clinical analysis of denture rehabilitation after mandibular fibula free-flap reconstruction [J]. Journal of Peking University (Health Sciences), 2024, 56(1): 66-73. |
| [11] | Sui LI,Wenjie MA,Shimin WANG,Qian DING,Yao SUN,Lei ZHANG. Trueness of different digital design methods for incisal guidance of maxillary anterior implant-supported single crowns [J]. Journal of Peking University (Health Sciences), 2024, 56(1): 81-87. |
| [12] | Xiaoqiang LIU,Yin ZHOU. Risk factors of perioperative hypertension in dental implant surgeries with bone augmentation [J]. Journal of Peking University (Health Sciences), 2024, 56(1): 93-98. |
| [13] | Da-wei WANG,Hua-dong WANG,Li LI,Xin YIN,Wei HUANG,Ji-dong GUO,Ya-feng YANG,Yi-hao LIU,Yang ZHENG. Efficacy analysis of autologous facet joint bone block in lumbar interbody fusion of osteoporosis patients [J]. Journal of Peking University (Health Sciences), 2023, 55(5): 899-909. |
| [14] | Qian DING,Wen-jin LI,Feng-bo SUN,Jing-hua GU,Yuan-hua LIN,Lei ZHANG. Effects of surface treatment on the phase and fracture strength of yttria- and magnesia-stabilized zirconia implants [J]. Journal of Peking University (Health Sciences), 2023, 55(4): 721-728. |
| [15] | Meng-en OU,Yun DING,Wei-feng TANG,Yong-sheng ZHOU. Three-dimensional finite element analysis of cement flow in abutment margin-crown platform switching [J]. Journal of Peking University (Health Sciences), 2023, 55(3): 548-552. |
|
||