Journal of Peking University (Health Sciences) ›› 2026, Vol. 58 ›› Issue (2): 372-379. doi: 10.19723/j.issn.1671-167X.2026.02.023
Previous Articles Next Articles
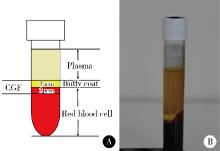
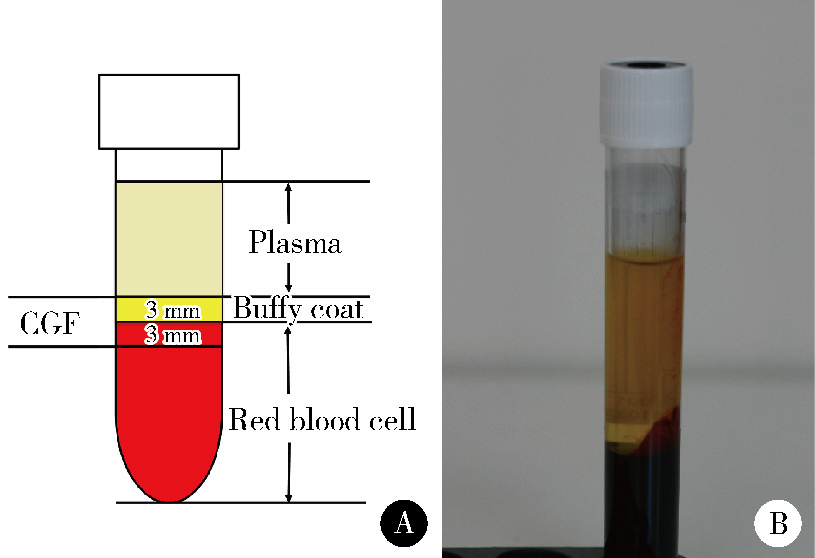
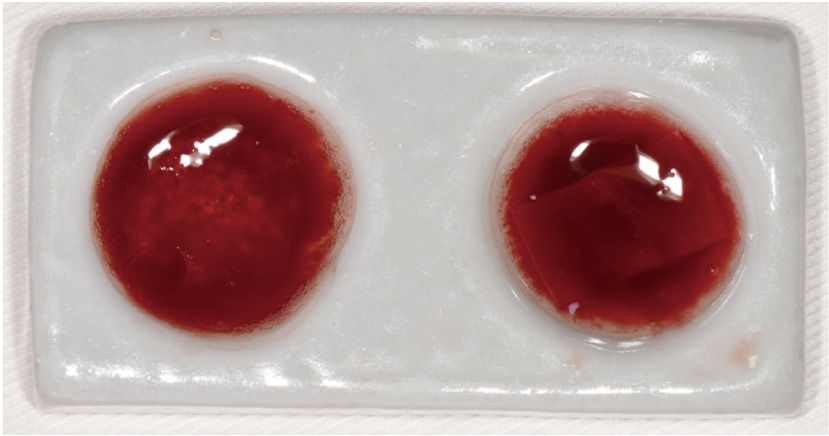
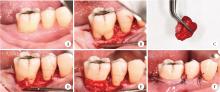
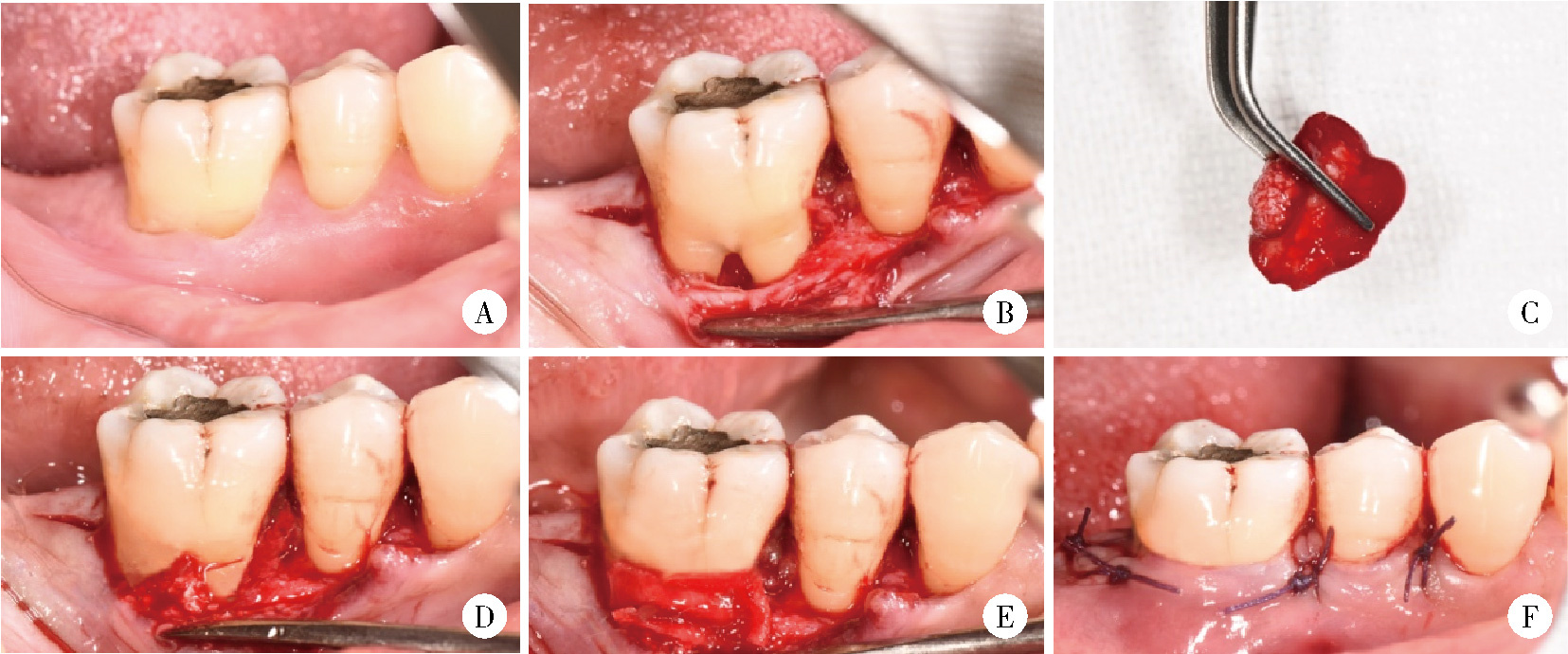
Effect of concentrated growth factors in guided tissue regeneration for the treatment of mandibular molar furcation lesions
Xinying WANG1, Xueyuan CHENG2, Mengjun ZHANG2, Fei LI2, Jinyu DUAN2, Jing QIAO2,*( )
)
- 1. Department of Oral and Maxillofacial Radiology, Peking University School and Hospital of Stomatology & National Cli-nical Research Center for Oral Diseases & National Engineering Laboratory for Digital and Material Technology of Stomatology & Beijing Key Laboratory of Digital Stomatology, Beijing 100081, China
2. First Clinical Division, Peking University School and Hospital of Stomatology, Beijing 100034, China
CLC Number:
- R781.4
| 1 |
doi: 10.1111/jcpe.14186 |
| 2 |
|
| 3 |
doi: 10.1177/0022034513496428 |
| 4 |
doi: 10.1111/jcmm.70374 |
| 5 |
doi: 10.2174/0115733998332692241202072249 |
| 6 |
|
| 7 |
doi: 10.1902/jop.2010.100306 |
| 8 |
doi: 10.11607/prd.2901 |
| 9 |
doi: 10.1111/jcpe.13238 |
| 10 |
doi: 10.4103/jisp.jisp_44_21 |
| 11 |
doi: 10.1111/j.1600-051X.2009.01428.x |
| 12 |
doi: 10.1902/jop.2011.100731 |
| 13 |
doi: 10.3390/jcm15020554 |
| 14 |
doi: 10.1111/odi.15325 |
| 15 |
doi: 10.1080/09537104.2016.1213381 |
| 16 |
doi: 10.1007/s00784-025-06673-y |
| 17 |
doi: 10.3390/ijms20061347 |
| 18 |
|
| 19 |
doi: 10.1002/jbm.a.36906 |
| 20 |
doi: 10.1002/jemt.20968 |
| 21 |
doi: 10.3892/mmr.2013.1756 |
| 22 |
|
| 23 |
doi: 10.1038/s41598-018-24364-5 |
| 24 |
doi: 10.1007/s00784-018-2582-z |
| [1] | Yue WANG, Yuhong LIANG. Florid cemento-osseous dysplasia: A case report [J]. Journal of Peking University (Health Sciences), 2026, 58(1): 220-224. |
| [2] | Shiyu QIU, Yang LIAN, Yifan KANG, Lei ZHANG, Yiwang CAI, Xiaofeng SHAN, Zhigang CAI. Personalized mandibular reconstruction assisted by three-dimensional retrieval model based on fully connected neural network and a database of mandibles [J]. Journal of Peking University (Health Sciences), 2025, 57(2): 360-368. |
| [3] | Fei WANG, Xinyue ZHANG, Muqing LIU, Enbo WANG, Denghui DUAN. Clinical application and three-dimensional finite element analysis of along-axis extraction method in mandibular mesial and horizontally impacted third molar surgery [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 106-112. |
| [4] | Yutong SHI, Yiping WEI, Wenjie HU, Tao XU, Haoyun ZHANG. Evaluation of micro crestal flap-alveolar ridge preservation following extraction of mandibular molars with severe periodontitis [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 33-41. |
| [5] | Xinying WANG, Xueyuan CHENG, Yong ZHANG, Fei LI, Jinyu DUAN, Jing QIAO. Therapeutic effect of concentrated growth factors combined with self-curing calcium phosphate cement on periodontal intrabony defects: Clinical and radiographic evaluation [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 42-50. |
| [6] | Chen CHEN,Yuhong LIANG. Root canal therapy of maxillary molars with atypical canals: A report of three cases [J]. Journal of Peking University (Health Sciences), 2024, 56(1): 190-195. |
| [7] | Deng-hui DUAN,Hom-Lay WANG,En-bo WANG. Role of collagen membrane in modified guided bone regeneration surgery using buccal punch flap approach: A retrospective and radiographical cohort study [J]. Journal of Peking University (Health Sciences), 2023, 55(6): 1097-1104. |
| [8] | Han LU,Jian-yun ZHANG,Rong YANG,Le XU,Qing-xiang LI,Yu-xing GUO,Chuan-bin GUO. Clinical factors affecting the prognosis of lower gingival squamous cell carcinoma [J]. Journal of Peking University (Health Sciences), 2023, 55(4): 702-707. |
| [9] | Zi-xiang GAO,Yong WANG,Ao-nan WEN,Yu-jia ZHU,Qing-zhao QIN,Yun ZHANG,Jing WANG,Yi-jiao ZHAO. Automatic determination of mandibular landmarks based on three-dimensional mandibular average model [J]. Journal of Peking University (Health Sciences), 2023, 55(1): 174-180. |
| [10] | TIAN Jing,QIN Man,CHEN Jie,XIA Bin. Early loss of primary molar and permanent tooth germ caused by the use of devitalizer during primary molar root canal therapy: Two cases report [J]. Journal of Peking University (Health Sciences), 2022, 54(2): 381-385. |
| [11] | CHEN Zhen,GU Bao-xin,TANG Yu-fang,YAN Zi-yu,NI Fang-duan,CUI Nian-hui. Constructions of the scale of difficulty in the extraction of impacted mandibular third molars by using Delphi method [J]. Journal of Peking University (Health Sciences), 2022, 54(1): 100-104. |
| [12] | Wei ZHOU,Jin-gang AN,Qi-guo RONG,Yi ZHANG. Three-dimensional finite element analysis of traumatic mechanism of mandibular symphyseal fracture combined with bilateral intracapsular condylar fractures [J]. Journal of Peking University (Health Sciences), 2021, 53(5): 983-989. |
| [13] | JIANG You-sheng,FENG Lin,GAO Xue-jun. Influence of base materials on stress distribution in endodontically treated maxillary premolars restored with endocrowns [J]. Journal of Peking University (Health Sciences), 2021, 53(4): 764-769. |
| [14] | Fei LI,Jing QIAO,Jin-yu DUAN,Yong ZHANG,Xiu-jing WANG. Effect of concentrated growth factors combined with guided tissue regeneration in treatment of classⅡ furcation involvements of mandibular molars [J]. Journal of Peking University (Health Sciences), 2020, 52(2): 346-352. |
| [15] | Shu-wen SHI,Yang MENG,Jian JIAO,Wen-jing LI,Huan-xin MENG,Qing-xian LUAN,Wan-chun WANG. Tooth loss and multivariable analysis after 5-year non-surgical periodontal treatment on molars with furcation involvement [J]. Journal of Peking University(Health Sciences), 2019, 51(5): 913-918. |
|
||