北京大学学报(医学版) ›› 2026, Vol. 58 ›› Issue (2): 332-336. doi: 10.19723/j.issn.1671-167X.2026.02.017
女性睾酮检测中假阳性问题及质谱法的确诊价值
- 1. 北京大学人民医院内分泌与代谢科, 北京 100044
2. 厦门市第三医院内分泌科, 福建厦门 361100
3. 北京大学糖尿病中心, 北京 100044
False positives in female testosterone testing and the diagnostic value of mass spectrometry
Man WU1,2, Yingying LUO1,3, Linong JI1,3,*( )
)
- 1. Department of Endocrinology and Metabolism, Peking University People's Hospital, Beijing 100044, China
2. Department of Endocrinology, The Third Hospital of Xiamen, Xiamen 361100, Fujian, China
3. Peking University Diabetes Center, Beijing 100044, China
摘要:
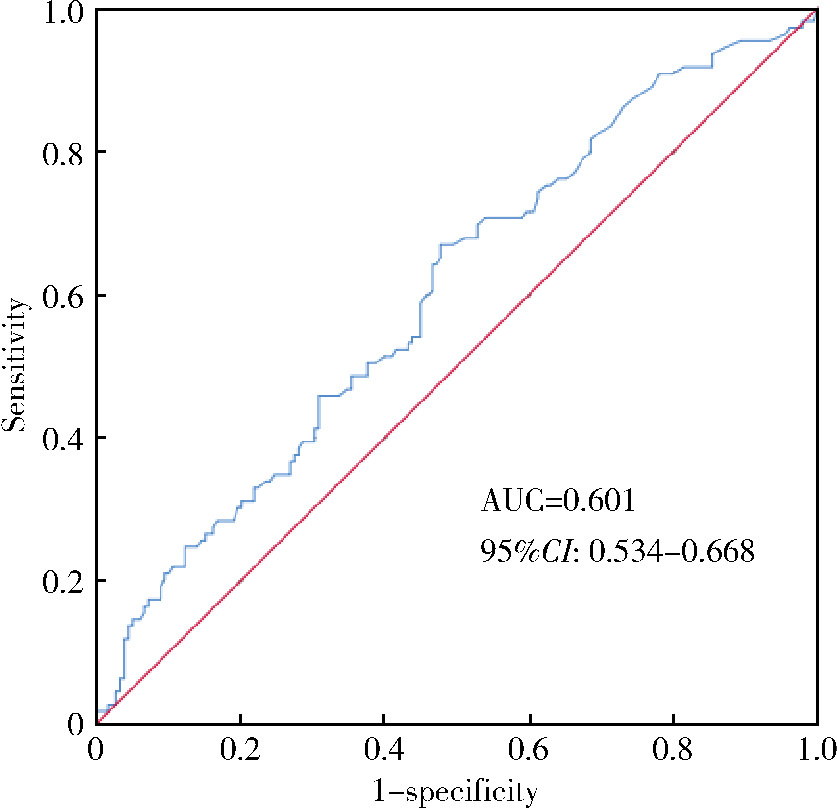
目的: 分析化学发光免疫分析法(chemiluminescence immunoassay, CLIA)测定女性睾酮水平假性升高的比例,并评估液相色谱-串联质谱法(liquid chromatography-tandem mass spectrometry,LC-MS/MS)在提高女性睾酮检测准确性中的应用价值。方法: 回顾性收集2020年1月1日至2024年5月1日就诊于北京大学人民医院,采用了CLIA检测睾酮水平升高并再次采集血样进行LC-MS/MS检测的女性患者。根据LC-MS/MS检测结果,将患者分为假性升高组和真性升高组,比较两组睾酮水平的差异,计算CLIA的假阳性率,并分析假性升高组进一步的检查情况。结果: 共纳入287例CLIA检测睾酮水平升高的女性患者,根据LC-MS/MS的结果,178例(62.0%)被归类为假性升高组,109例(38.0%)被归类为真性升高组,两组睾酮水平(CLIA检测结果)的均值分别为(3.63±1.60) nmol/L和(4.13±2.20) nmol/L,差异有统计学意义(P < 0.05)。CLIA检测女性睾酮水平的假阳性率为62.0%,受试者工作特征(receiver operating characteristic, ROC)曲线下面积(area under the curve,AUC)为0.601(95%CI:0.534~0.668),提示其诊断准确性较低。假性升高组中,40.45%的患者接受了多次CLIA复测,部分患者接受了不必要的临床评估,包括影像学和激素检查,增加了患者负担。结论: CLIA在女性睾酮检测中的假阳性率较高,假阳性结果可能导致误诊、重复检测和不必要的其他相关检查,增加了患者负担和医疗资源浪费;LC-MS/MS可显著提高女性睾酮水平评估的准确性,建议在CLIA检测睾酮水平升高的女性患者中优先采用LC-MS/MS进行确诊。
中图分类号:
- R588
| 1 |
doi: 10.1016/S2213-8587(22)00163-2 |
| 2 |
doi: 10.1210/clinem/dgae302 |
| 3 |
doi: 10.1016/0002-9378(92)91779-A |
| 4 |
doi: 10.1093/humrep/dex078 |
| 5 |
doi: 10.1530/EC-18-0450 |
| 6 |
doi: 10.1016/j.cca.2019.11.003 |
| 7 |
doi: 10.1016/j.molmet.2020.01.001 |
| 8 |
doi: 10.1210/clinem/dgab275 |
| 9 |
|
| 10 |
doi: 10.1016/j.fertnstert.2008.06.035 |
| 11 |
|
| 12 |
doi: 10.3390/biom10121697 |
| 13 |
doi: 10.1210/jc.2006-1864 |
| 14 |
doi: 10.1016/j.maturitas.2010.04.019 |
| 15 |
doi: 10.1530/EJE-11-1051 |
| 16 |
|
| 17 |
doi: 10.1016/j.beem.2022.101665 |
| 18 |
|
| 19 |
|
| 20 |
doi: 10.1210/jc.2015-2807 |
| 21 |
doi: 10.1016/j.steroids.2018.09.001 |
| 22 |
尹逸丛, 卢琳, 朱惠娟, 等. 女性睾酮水平假性升高病例的临床特点和检验验证[J]. 生殖医学杂志, 2021, 30 (7): 852- 857.
|
| 23 |
中华医学会妇产科学分会内分泌学组及指南专家组. 多囊卵巢综合征中国诊疗指南[J]. 中华妇产科杂志, 2018, 53 (1): 2- 6.
|
| 24 |
doi: 10.1210/clinem/dgad463 |
| 25 |
曹正, 阮祥燕, 翟燕红, 等. 多囊卵巢综合征雄激素质谱检测专家共识[J]. 检验医学, 2023, 38 (3): 203- 208.
|
| 26 |
doi: 10.1016/j.maturitas.2019.04.203 |
| [1] | 花克涵,杨磊,张晓威,白文俊,李清,徐涛. 完全性雄激素不敏感综合征合并膀胱瘘1例报道及文献回顾[J]. 北京大学学报(医学版), 2017, 49(4): 724-729. |
| [2] | 伏海燕, 靖俊, 伊男, 余时超, 恽时峰, 梁元姣, 姚兵. StarD7与Wnt/β-catenin信号通路对Annexin 5刺激大鼠Leydig细胞睾酮分泌的影响[J]. 北京大学学报(医学版), 2012, 44(4): 518-523. |
| [3] | 陈亮, 徐阳 , 左文莉 , 杨慧霞, 廖秦平, 辛钟成, 郭应禄. Ras分子信号蛋白调控睾丸间质细胞Cox7a2蛋白表达及共定位影响研究[J]. 北京大学学报(医学版), 2012, 44(4): 507-510. |
|
||