Journal of Peking University (Health Sciences) ›› 2024, Vol. 56 ›› Issue (5): 896-901. doi: 10.19723/j.issn.1671-167X.2024.05.022
Previous Articles Next Articles
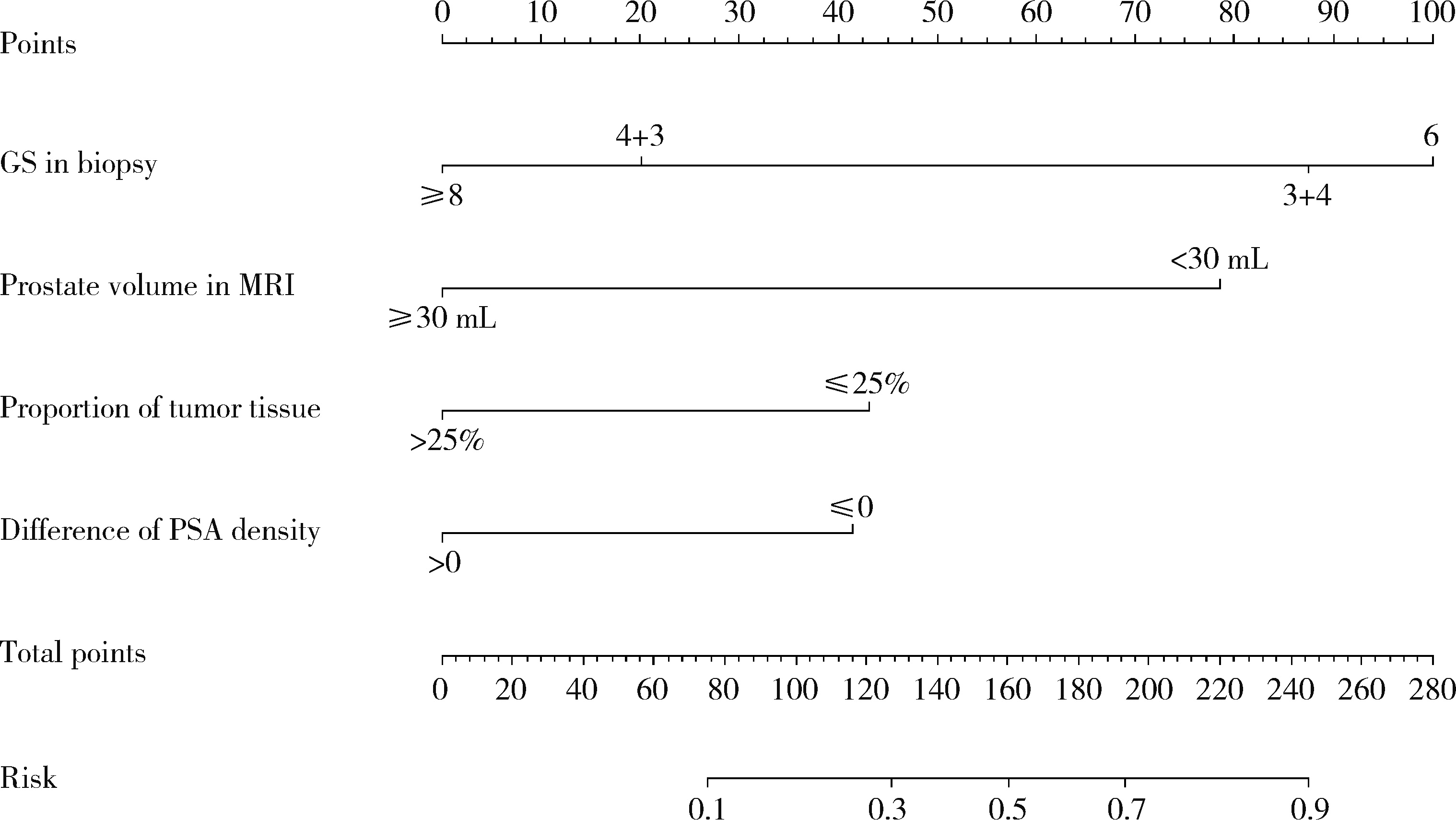
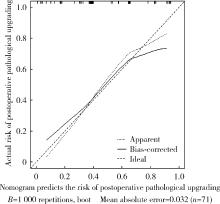
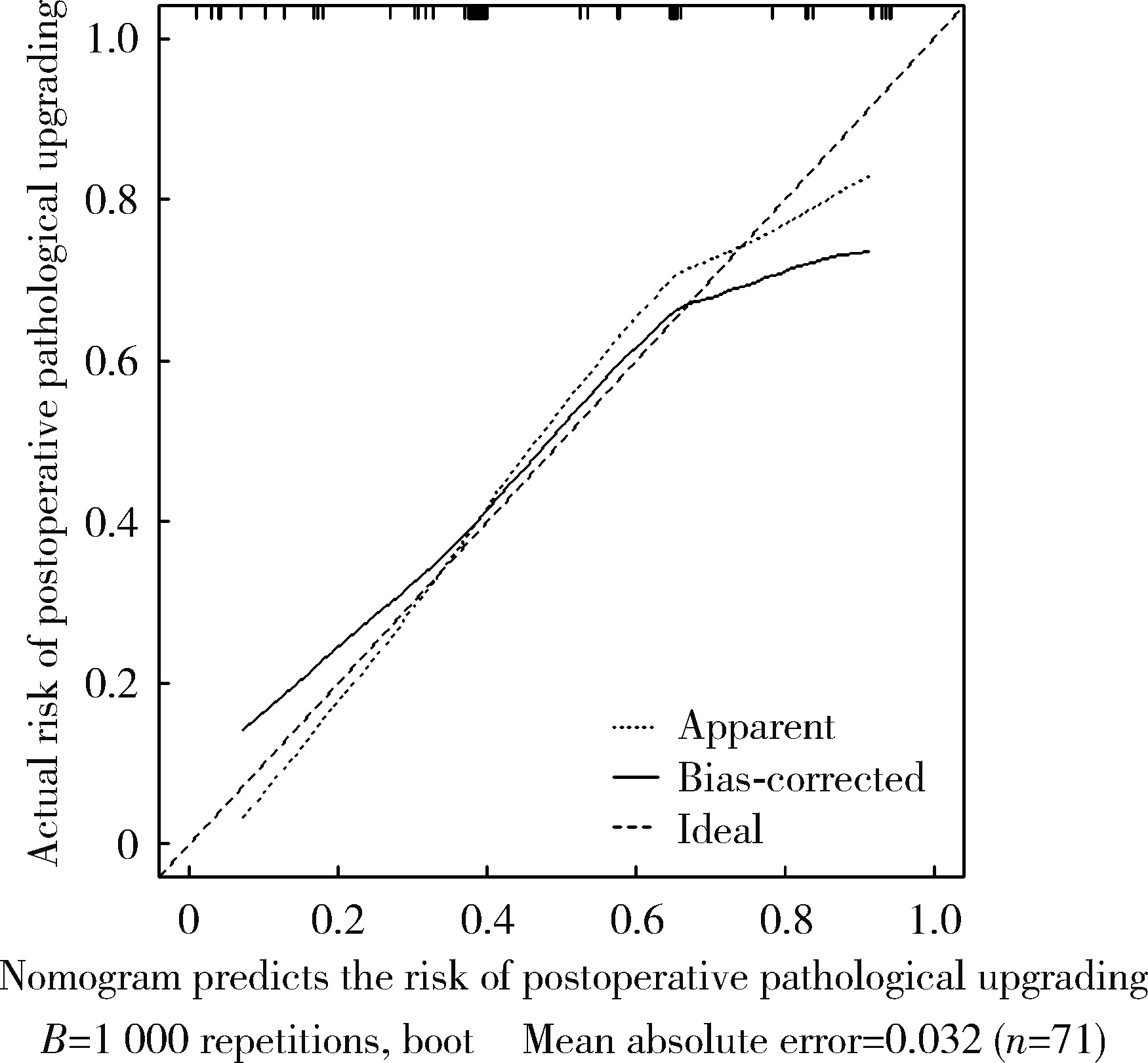
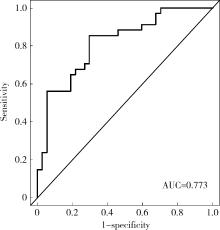
Risk factors analysis and nomogram model construction of postoperative pathological upgrade of prostate cancer patients with single core positive biopsy
Zhicun LI, Tianyu WU, Lei LIANG, Yu FAN, Yisen MENG*( ), Qian ZHANG*(
), Qian ZHANG*( )
)
- Department of Urology, Peking University First Hospital; Institution of Urology, Peking University; Beijing Key Laboratory of Urogenital Diseases (Male) Molecular Diagnosis and Treatment Center; National Urological Cancer Center, Beijing 100034, China
CLC Number:
- R737.25
| 1 | 郑荣寿, 陈茹, 韩冰峰, 等. 2022年中国恶性肿瘤流行情况分析[J]. 中华肿瘤杂志, 2024, 46 (3): 221- 231. |
| 2 |
Siegel RL , Miller KD , Jemal A . Cancer statistics, 2020[J]. CA Cancer J Clin, 2020, 70 (1): 7- 30.
doi: 10.3322/caac.21590 |
| 3 | 徐毅, 毛祺琦, 刘犇, 等. 穿刺单针阳性前列腺癌的术后病理特征分析[J]. 中华泌尿外科杂志, 2018, 39 (10): 757- 760. |
| 4 | 陈小豹, 张潮鸿, 江玮, 等. 前列腺穿刺单针阳性的临床特点[J]. 中国男科学杂志, 2019, 33 (3): 30- 33. |
| 5 | 唐超来, 唐贤富, 郑兴明. 前列腺穿刺活检单针阳性患者行前列腺根治性切除术后的病理特征[J]. 国际泌尿系统杂志, 2020, 40 (4): 587- 590. |
| 6 |
Goldstein NS , Bégin LR , Grody WW , et al. Minimal or no cancer in radical prostatectomy specimens. Report of 13 cases of the "vanishing cancer phenomenon"[J]. Am J Surg Pathol, 1995, 19 (9): 1002- 1009.
doi: 10.1097/00000478-199509000-00003 |
| 7 |
Ricardo Kupka da S , Dall'Oglio MF , Sant'Ana AC , et al. Can single positive core prostate cancer at biopsy be considered a low-risk disease after radical prostatectomy?[J]. Int Braz J Urol, 2013, 39 (6): 800- 807.
doi: 10.1590/S1677-5538.IBJU.2013.06.05 |
| 8 | 刘希高, 谌诚, 李健, 等. 前列腺穿刺活检单针阳性患者前列腺内癌灶分布特点[J]. 中华男科学杂志, 2012, 18 (2): 155- 159. |
| 9 | 杜少静, 贺慧颖. 穿刺单针阳性前列腺癌患者根治术后62例临床病理分析[J]. 中华病理学杂志, 2016, 45 (7): 446- 450. |
| 10 |
郝一昌, 颜野, 张帆, 等. 穿刺活检单针阳性的前列腺癌手术策略选择及经验总结[J]. 北京大学学报(医学版), 2020, 52 (4): 625- 631.
doi: 10.19723/j.issn.1671-167X.2020.04.005 |
| 11 | Dong F , Jones JS , Stephenson AJ , et al. Prostate cancer volume at biopsy predicts clinically significant upgrading[J]. J Urol, 2008, 179 (3): 896- 900. |
| 12 | Hwang I , Lim D , Jeong YB , et al. Upgrading and upstaging of low-risk prostate cancer among Korean patients: A multicenter study[J]. Asian J Androl, 2015, 17 (5): 811- 814. |
| [1] | Hui WEI, Jingfeng ZHANG, Zhongqiang YAO, Jinxia ZHAO. Clinical characteristics and relevant factors of rheumatoid arthritis patients with anemia of chronic disease [J]. Journal of Peking University (Health Sciences), 2026, 58(2): 307-312. |
| [2] | Jie ZHAO, Chun FU, Xiujuan ZHAO, Haiyan XUE, Shu LI, Zhenzhou WANG, Fengxue ZHU. Risk factors for ventilator-associated pneumonia in patients with chest trauma in intensive care unit [J]. Journal of Peking University (Health Sciences), 2026, 58(2): 351-358. |
| [3] | Yanhua LIU, Min LU, Xuyang ZHAO, Kuan'gen ZHANG, Rui WU, Fang MEI, Zhihao DAI, Jiangfeng YOU, Fei PEI. Effect of dephosphorylation of tumor metastasis suppressor gene LASS2 on vacuolar ATPase activity and invasiveness of prostate cancer [J]. Journal of Peking University (Health Sciences), 2025, 57(6): 1113-1123. |
| [4] | Bowen LI, Qiang ZHANG, Yixin SUN. Establishment and validation of a risk prediction model for scoliosis after Nuss procedure in children and young adults with pectus excavatum [J]. Journal of Peking University (Health Sciences), 2025, 57(5): 941-946. |
| [5] | Xiaoyong YANG, Fan ZHANG, Lulin MA, Cheng LIU. Clinical characteristics and influencing factors of extraglandular invasion of prostatic ductal adenocarcinoma [J]. Journal of Peking University (Health Sciences), 2025, 57(5): 956-960. |
| [6] | Jiaxin NING, Haoran WANG, Shuhang LUO, Jibo JING, Jianye WANG, Huimin HOU, Ming LIU. Multi-omics analysis of the relationship between oxidative stress-related gene and prostate cancer [J]. Journal of Peking University (Health Sciences), 2025, 57(4): 633-643. |
| [7] | Zeyuan WANG, Shuanbao YU, Haoke ZHENG, Jin TAO, Yafeng FAN, Xuepei ZHANG. A preoperative prediction model for pelvic lymph node metastasis in prostate cancer: Integrating clinical characteristics and multiparametric MRI [J]. Journal of Peking University (Health Sciences), 2025, 57(4): 684-691. |
| [8] | Wei LIU, Wen GUO, Zhe GUO, Chunyan LI, Yunlong LI, Siqi LIU, Liang ZHANG, Hui SONG. Risk factors associated with non-radiographic bone erosion in patients with gout [J]. Journal of Peking University (Health Sciences), 2025, 57(4): 735-739. |
| [9] | Mengxi LU, Qiuping LIU, Tianjing ZHOU, Xiaofei LIU, Yexiang SUN, Peng SHEN, Hongbo LIN, Xun TANG, Pei GAO. Association of triglyceride-glucose index and cardiovascular disease in a community-based Chinese cohort [J]. Journal of Peking University (Health Sciences), 2025, 57(3): 430-435. |
| [10] | Huaqiu GUO, Zhe WANG, Xue YANG, Jie BAI. Clinical features and risk factors of patients with oral bleeding in dental emergency [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 142-147. |
| [11] | Minting DENG, Nan WANG, Bin XIA, Yuming ZHAO, Junxia ZHU. Factors associated with spontaneous re-eruption of traumatically intruded permanent anterior teeth in children and adolescents [J]. Journal of Peking University (Health Sciences), 2025, 57(1): 148-153. |
| [12] | Yukai LI, Hongyan WANG, Liang LUO, Yun LI, Chun LI. Clinical significance of antiphospholipid antibodies in Behcet disease with thrombosis [J]. Journal of Peking University (Health Sciences), 2024, 56(6): 1036-1040. |
| [13] | Yang TIAN, Yongzheng HAN, Jiao LI, Mingya WANG, Yinyin QU, Jingchao FANG, Hui JIN, Min LI, Jun WANG, Mao XU, Shenglin WANG, Xiangyang GUO. Incidence and risk factors of postoperative epidural hematoma following anterior cervical spine surgery [J]. Journal of Peking University (Health Sciences), 2024, 56(6): 1058-1064. |
| [14] | Mingrui WANG, Jinhui LAI, Jiaxiang JI, Xinwei TANG, Haopu HU, Qi WANG, Kexin XU, Tao XU, Hao HU. Risk factors for decreased quality of life in patients with kidney stones predicted by the Chinese version of Wisconsin stone quality of life questionnaire [J]. Journal of Peking University (Health Sciences), 2024, 56(6): 1069-1074. |
| [15] | Yuanmei LIU, Yicheng FU, Jingxin HAO, Fuchun ZHANG, Huilin LIU. Construction and validation of a nomogram for predicting in-hospital postoperative heart failure in elderly patients with hip fracture [J]. Journal of Peking University (Health Sciences), 2024, 56(5): 874-883. |
|
||