北京大学学报(医学版) ›› 2020, Vol. 52 ›› Issue (2): 281-284. doi: 10.19723/j.issn.1671-167X.2020.02.014
Friedman分型联合术后早期睡眠脉氧监测对悬雍垂腭咽成形术疗效的预测价值
- 北京大学第一医院耳鼻咽喉头颈外科,北京 100034
Predictive values of the combination of Friedman stage and sleep oximetry done early after surgery in predicting the treatment outcomes of uvulopalatopharyngoplasty
Bing-wan DONG,Jun-bo ZHANG,Shui-fang XIAO( )
)
- Department of Otorhinolaryngology Head and Neck Surgery, Peking University First Hospital, Beijing 100034, China
摘要:
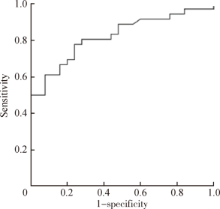
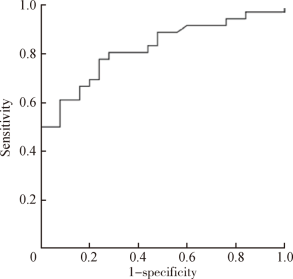
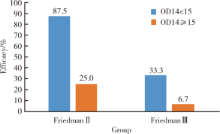
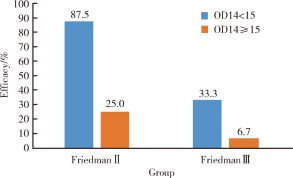
目的 探讨阻塞性睡眠呼吸暂停低通气综合征(obstructive sleep apnea hypopnea syndrome,OSAHS)患者术前病史及查体等资料,联合术后早期睡眠血氧结果,对悬雍垂腭咽成形术(uvulopalatopharyngoplasty,UPPP)疗效的预测价值.方法: 选择2013年1月至2016年5月于北京大学第一医院接受UPPP手术治疗且有完整随访资料的患者进行回顾性研究,搜集包括年龄,查体及睡眠监测等资料,所有患者在术后早期(1周)均实施主观疗效评估及整夜脉氧监测,术后长期疗效评估进行至少术后3个月的睡眠监测及视觉模拟量表评估.结果: 共纳入61 例患者,完成随访后有效者25 例(41.0%), 无效者36 例(59.0%), 回归分析发现术后早期≥4%的氧降指数(the oxygen index of ≥4%,ODI4)及术前Friedman分型是疗效的独立预测参数(P<0.05),ROC曲线分析术后早期ODI4对疗效的预测效率,发现曲线下面积可达0.822,以15作为界值,敏感性和特异性分别可达0.778和0.760,其中ODI4<15 次/h的患者有效率可达70.4%,显著高于ODI4≥15 次/h的患者,即17.6%(P<0.05);术前Friedman分型Ⅱ型患者中,ODI4<15次/h的患者,其有效率显著高于ODI4≥15 次/h的患者(87.5% vs. 25.0%),Ⅲ型患者中亦可得到类似的结果(33.3% vs. 6.7%).结论: 通过对UPPP术后早期脉氧监测数据尤其是ODI4的收集,结合术前的Friedman分型,能更好地判断患者潜在的手术疗效.
中图分类号:
- R766.9
| [1] | 中国医师协会睡眠医学专业委员会. 成人阻塞性睡眠暂停多学科诊疗指南[J]. 中华医学杂志, 2018,98(24):1902-1914. |
| [2] | Borowiecki BD, Sassin JF . Surgical treatment of sleep apnea[J]. Arch Otolaryngol, 1983,109(8):506-512. |
| [3] | Friedman M, Landsberg R, Tanyeri H . Submucosal uvulopalatopharyngoplasty[J]. Otolaryngol Head Neck Surg, 2000,11(1):26-29. |
| [4] | Friedman M, Ibrahim H, Joseph NJ . Staging of obstructive sleep apnea/hypopnea syndrome: a guide to appromiate treatment[J]. Laryngoscope, 2004,114(3):454-459. |
| [5] | Friedman M ,I brahim H, Bass L.Clinical staging for sleep-disordered breathing[J]. Otolaryngol Head Neck Surg, 2002,127(1):13-21. |
| [6] | Liu JM, Yi B, Ye JY . Combination of transpalatal advancement pharyngoplasty and H-uvulopalatopharyngoplasty for obstructive sleep apnea[J]. Oper Tech Otolayngol Head Neck Surg, 2009,20(2):152-158. |
| [7] | Iwanaga K, Hasegawa K, Shibata N , et al. Endoscopic examination of obstructive sleep apnea syndrome patients during drug-induced sleep[J].Acta Otolaryngol Suppl, 2003(550):36-40. |
| [8] | Sanders MH, Johnson JT, Keller F , et al. The acute effects of uvulopalatopharyngoplasty on breathing during sleep in sleep apnea patients[J]. Sleep, 1988,11(1):75-89. |
| [9] | Weaver EM, Woodson BT, Yueh B , et al. Studying life effect & effectiveness of palatopharyngoplasty (SLEEP) study: subjective outcomes of isolated uvulopalatopharyngoplasty[J]. Otolaryngol Head Neck Surg, 2011,144(4):623-631. |
| [10] | Kezirian EJ, Weaver EM, Criswell MA , et al. Reporting results of obstructive sleep apnea syndrome surgery trials[J]. Otolaryngol Head Neck Surg, 2011,144(4):496-499. |
| [11] | Dickson RI, Blokmanis A . Treatment of obstructive sleep apnea by uvulopalatopharyngoplasty[J]. Laryngoscope, 1987,97(9):1054-1059. |
| [12] | Corcoran S, Mysliwiec V, Niven AS , et al. Development of central sleep apnea after maxillofacial surgery for obstructive sleep apnea[J]. J Clin Sleep Med, 2009,5(2):151-153. |
| [13] | Sanders MH, Costantino JP, Johnson JT . Polysomnography early after uvulopalatopharyngoplasty as a predictor of late postoperative results[J]. Chest, 1990,97(4):913-919. |
| [14] | Zhang JB, Li YR, Cao X , et al. The combination of anatomy and physiology in predicting the outcomes of velopharyngeal surgery[J]. Laryngoscope, 2014,124:1718-1723. |
| [15] | He M . Long-term efficacy of uvulopalatopharyngoplasty among adult patients with obstructive sleep apnea: a systematic review and meta-analysis[J]. Otolaryngol Head Neck Surg, 2019,161(3):401-411. |
| [16] | Choi JH, Cho SH, Kim SN , et al. Predicting outcomes after Uvulopalatopharyngoplasty for adult obstructive sleep apnea: a meta-analysis[J]. Otolaryngol Head Neck Surg, 2016,155(6):904-913. |
| No related articles found! |
|
||