北京大学学报(医学版) ›› 2026, Vol. 58 ›› Issue (2): 372-379. doi: 10.19723/j.issn.1671-167X.2026.02.023
浓缩生长因子联合引导性组织再生术治疗下颌磨牙根分叉病变的疗效
王昕莹1,*, 程雪原2,*, 张孟钧2, 李菲2, 段晋瑜2, 乔静2,*( )
)
- 1. 北京大学口腔医学院·口腔医院医学影像科, 国家口腔医学中心, 国家口腔疾病临床医学研究中心, 口腔生物材料和数字诊疗装备国家工程研究中心, 北京 100081
2. 北京大学口腔医学院·口腔医院门诊部, 北京 100034
Effect of concentrated growth factors in guided tissue regeneration for the treatment of mandibular molar furcation lesions
Xinying WANG1, Xueyuan CHENG2, Mengjun ZHANG2, Fei LI2, Jinyu DUAN2, Jing QIAO2,*( )
)
- 1. Department of Oral and Maxillofacial Radiology, Peking University School and Hospital of Stomatology & National Cli-nical Research Center for Oral Diseases & National Engineering Laboratory for Digital and Material Technology of Stomatology & Beijing Key Laboratory of Digital Stomatology, Beijing 100081, China
2. First Clinical Division, Peking University School and Hospital of Stomatology, Beijing 100034, China
摘要:
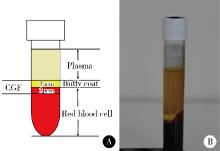
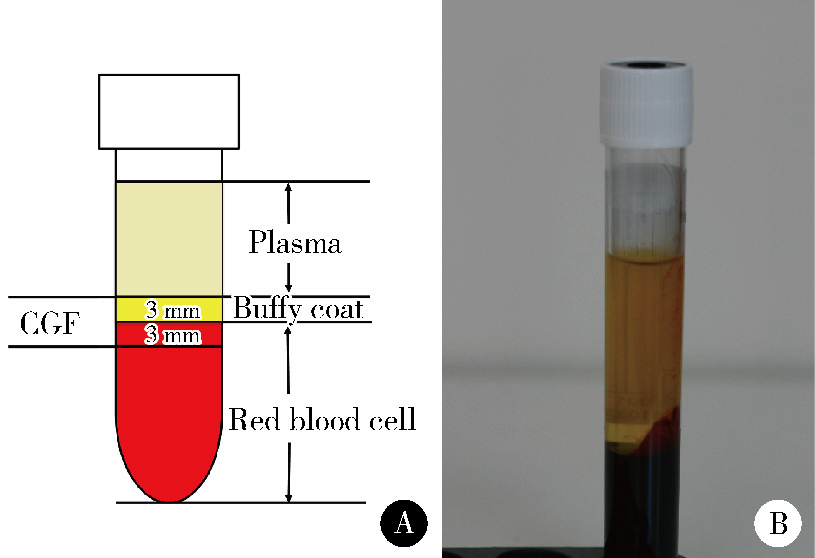
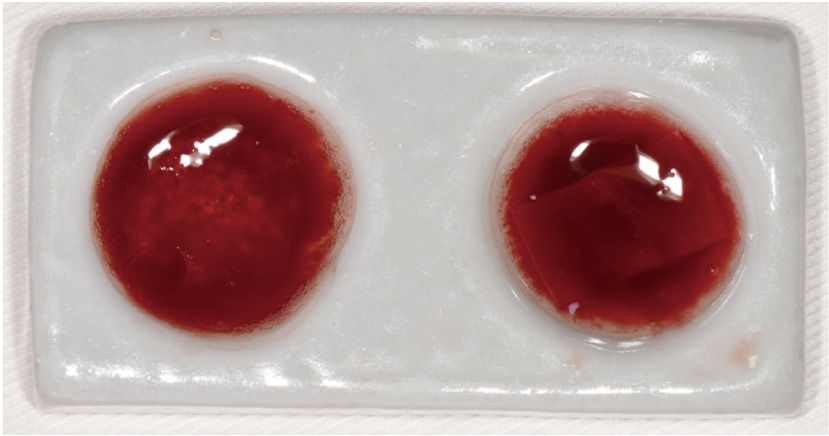
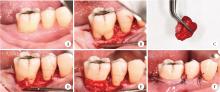
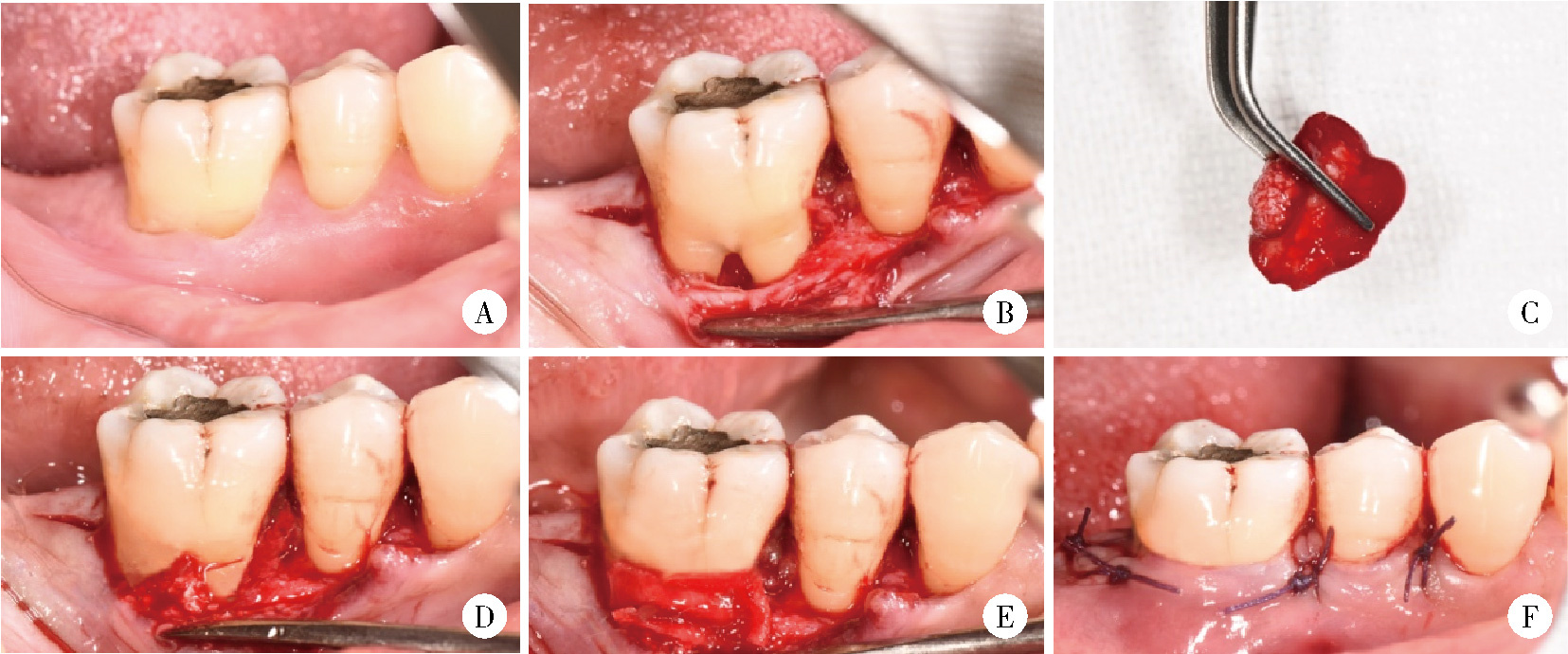
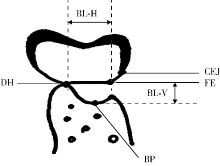
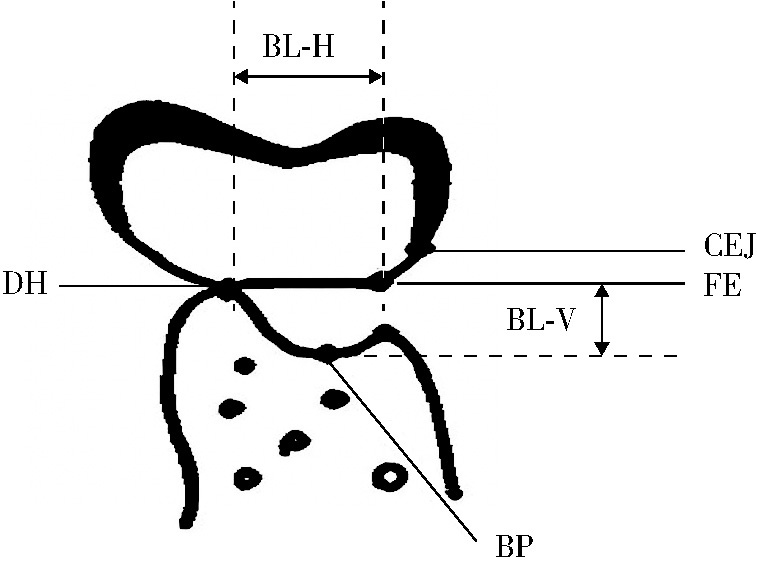
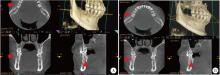
目的: 评价浓缩生长因子(concentrated growth factors,CGF)促进引导性组织再生术(guided tissue regeneration,GTR)联合植骨术治疗下颌磨牙Ⅱ度根分叉病变的临床效果,为根分叉病变的再生寻求更好的治疗方法。方法: 纳入16例需进行牙周手术的慢性牙周炎患者(共20颗下颌磨牙,含36例颊舌侧Ⅱ度根分叉病变),随机分为两组(每组18例病变),试验组采用GTR+植骨术+CGF进行治疗,对照组采用GTR+植骨术进行治疗。分别于术前、术后6个月和1年对患牙进行临床检查,并拍摄锥形束CT(cone beam CT,CBCT)。比较试验组和对照组手术前后临床和CBCT数据的变化。结果: 基线时两组的探诊深度、垂直和水平附着丧失,以及CBCT所示的垂直向和水平向骨丧失差异均无统计学意义(P>0.05)。术后6个月和1年时两组的临床指标及术后1年时两组的CBCT指标较基线时均有显著改善(P < 0.01),且试验组改善程度显著优于对照组(P < 0.05)。其中,术后1年时试验组探诊深度减少(4.75±1.87) mm,垂直和水平附着丧失分别减少(5.55±1.04) mm和(3.89±1.22) mm;对照组探诊深度减少(3.43±1.76) mm,垂直和水平附着丧失分别减少(4.41±1.08) mm和(3.07±1.02) mm。CBCT显示,试验组垂直向和水平向骨丧失分别减少(4.05±1.37) mm和(4.02±1.32) mm,对照组分别减少(3.17±1.09) mm和(3.27±1.08) mm。结论: 为期1年的观察结果显示,CGF可以促进GTR+植骨术在下颌磨牙Ⅱ度根分叉病变中的再生治疗效果。
中图分类号:
- R781.4
| 1 |
doi: 10.1111/jcpe.14186 |
| 2 |
|
| 3 |
doi: 10.1177/0022034513496428 |
| 4 |
doi: 10.1111/jcmm.70374 |
| 5 |
doi: 10.2174/0115733998332692241202072249 |
| 6 |
|
| 7 |
doi: 10.1902/jop.2010.100306 |
| 8 |
doi: 10.11607/prd.2901 |
| 9 |
doi: 10.1111/jcpe.13238 |
| 10 |
doi: 10.4103/jisp.jisp_44_21 |
| 11 |
doi: 10.1111/j.1600-051X.2009.01428.x |
| 12 |
doi: 10.1902/jop.2011.100731 |
| 13 |
doi: 10.3390/jcm15020554 |
| 14 |
doi: 10.1111/odi.15325 |
| 15 |
doi: 10.1080/09537104.2016.1213381 |
| 16 |
doi: 10.1007/s00784-025-06673-y |
| 17 |
doi: 10.3390/ijms20061347 |
| 18 |
|
| 19 |
doi: 10.1002/jbm.a.36906 |
| 20 |
doi: 10.1002/jemt.20968 |
| 21 |
doi: 10.3892/mmr.2013.1756 |
| 22 |
|
| 23 |
doi: 10.1038/s41598-018-24364-5 |
| 24 |
doi: 10.1007/s00784-018-2582-z |
| [1] | 王月, 梁宇红. 繁茂型牙骨质-骨结构不良1例[J]. 北京大学学报(医学版), 2026, 58(1): 220-224. |
| [2] | 仇师禹, 练洋, 康一帆, 张雷, 蔡义望, 单小峰, 蔡志刚. 基于下颌骨数据库和全连接神经网络的三维检索模型辅助下的下颌骨个性化重建[J]. 北京大学学报(医学版), 2025, 57(2): 360-368. |
| [3] | 王菲, 张馨月, 刘木清, 王恩博, 段登辉. 顺牙长轴拔牙法在下颌近中与水平智齿拔除术中的应用及三维有限元分析[J]. 北京大学学报(医学版), 2025, 57(1): 106-112. |
| [4] | 石宇彤, 危伊萍, 胡文杰, 徐涛, 张浩筠. 罹患重度牙周炎下颌磨牙拔牙微翻瓣牙槽嵴保存效果评价[J]. 北京大学学报(医学版), 2025, 57(1): 33-41. |
| [5] | 王昕莹, 程雪原, 张勇, 李菲, 段晋瑜, 乔静. 浓缩生长因子与自固化磷酸钙人工骨联合治疗牙周骨下袋缺损的疗效:临床和影像学评价[J]. 北京大学学报(医学版), 2025, 57(1): 42-50. |
| [6] | 康一帆, 葛严军, 吕晓鸣, 谢尚, 单小峰, 蔡志刚. 即刻种植体支持式义齿修复的血管化髂骨瓣重建下颌骨缺损[J]. 北京大学学报(医学版), 2025, 57(1): 78-84. |
| [7] | 李红光,韩玮华,吴训,冯继玲,李刚,孟娟红. 关节腔冲洗联合液态浓缩生长因子注射治疗单侧颞下颌关节骨关节炎的初步研究[J]. 北京大学学报(医学版), 2024, 56(2): 338-344. |
| [8] | 陈晨,梁宇红. 复杂根管上颌磨牙的根管治疗3例[J]. 北京大学学报(医学版), 2024, 56(1): 190-195. |
| [9] | 徐心雨,吴灵,宋凤岐,李自力,张益,刘筱菁. 基于下颌运动轨迹的正颌外科术中下颌骨髁突定位方法及初步精度验证[J]. 北京大学学报(医学版), 2024, 56(1): 57-65. |
| [10] | 王聪伟,高敏,于尧,章文博,彭歆. 游离腓骨瓣修复下颌骨缺损术后义齿修复的临床分析[J]. 北京大学学报(医学版), 2024, 56(1): 66-73. |
| [11] | 卢汉,张建运,杨榕,徐乐,李庆祥,郭玉兴,郭传瑸. 下颌牙龈鳞状细胞癌患者预后的影响因素[J]. 北京大学学报(医学版), 2023, 55(4): 702-707. |
| [12] | 雷玥,杨颖婷,雷海华. 异位萌出诱导矫治器在第一恒磨牙异位萌出治疗中的应用[J]. 北京大学学报(医学版), 2023, 55(4): 766-封三. |
| [13] | 高梓翔,王勇,温奥楠,朱玉佳,秦庆钊,张昀,王晶,赵一姣. 基于三维下颌骨平均模型的颌骨标志点自动确定方法[J]. 北京大学学报(医学版), 2023, 55(1): 174-180. |
| [14] | 田靖,秦满,陈洁,夏斌. 失活剂烧伤致乳磨牙早失及恒牙胚丧失2例[J]. 北京大学学报(医学版), 2022, 54(2): 381-385. |
| [15] | 陈震,谷宝鑫,汤玉芳,闫子玉,倪方端,崔念晖. 应用Delphi法构建下颌阻生第三磨牙拔除难度评分量表[J]. 北京大学学报(医学版), 2022, 54(1): 100-104. |
|
||