北京大学学报(医学版) ›› 2021, Vol. 53 ›› Issue (1): 120-125. doi: 10.19723/j.issn.1671-167X.2021.01.018
玻璃体和通用型复合树脂耐磨性的临床对照研究
- 1.北京大学口腔医学院·口腔医院,牙体牙髓科 国家口腔疾病临床医学研究中心 口腔数字化医疗技术和材料国家工程实验室 口腔数字医学北京市重点实验室,北京 100081
2.北京大学口腔医学院·口腔医院第一门诊部综合科,北京 100034
Evaluation of wear property of Giomer and universal composite in vivo
MU Hai-li1,2,TIAN Fu-cong3,WANG Xiao-yan1,Δ( ),GAO Xue-jun1
),GAO Xue-jun1
- 1. Department of Cariology and Endodontology, Peking University School and Hospital of Stomatology & National Clinical Research Center for Oral Diseases & National Engineering Laboratory for Digital and Material Technology of Stomatology & Beijing Key Laboratory of Digital Stomatology, Beijing 100081, China
2. First Clinical Division, Peking University School and Hospital of Stomatology, Beijing 100034, China
摘要:
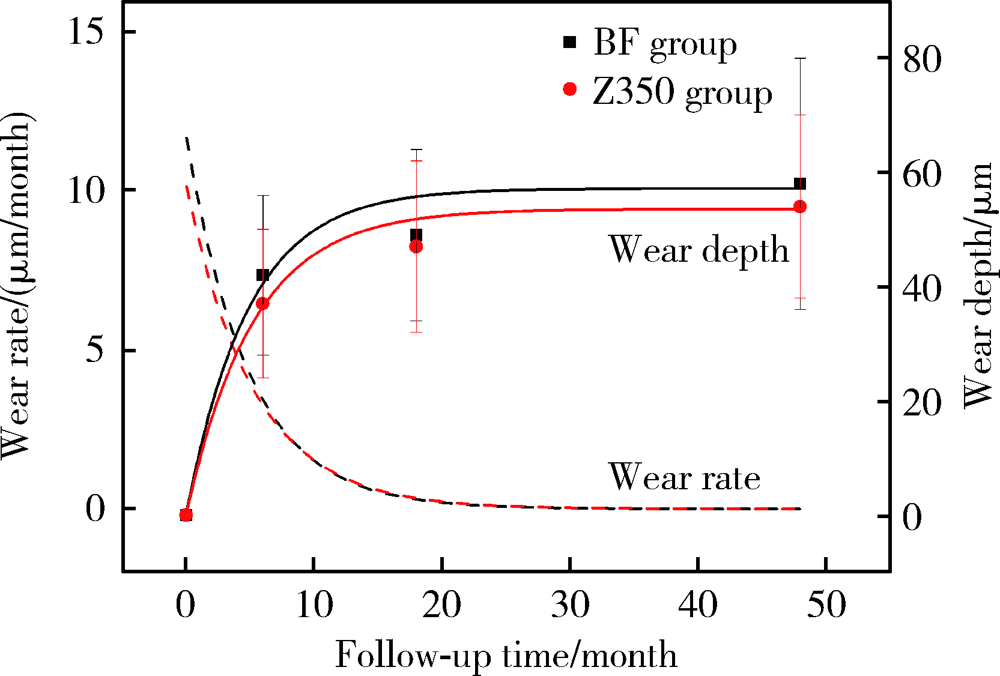
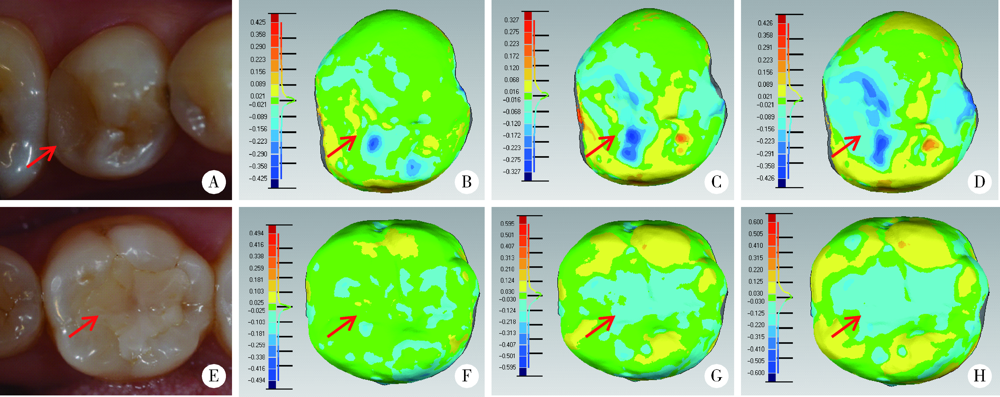
目的: 采用激光三维扫描技术评估玻璃体和通用型复合树脂用于后牙充填的耐磨性。方法: 根据纳入标准选取48名患者共108颗患牙(每组各54颗),随机分配用玻璃体(Beautifil Ⅱ,简称BF)或通用型复合树脂(Filtek Z350,简称Z350)进行充填。分别于术后1周、6个月、18个月和4年,采用改良美国公共卫生署(United States Public Health Service,USPHS)标准对充填体进行临床评价并拍照和制取模型。使用激光三维扫描仪扫描模型后,对图像进行配准和计算磨耗深度,使用SPSS 20.0进行统计分析。结果: 术后4年回访43名患者,回访率为89.6%。BF组和Z350组各有4例和3例出现脱落、继发龋、充填体折断和牙髓坏死。两组充填体的4年存留率均为95.8%,符合美国牙医协会(American Dental Association,ADA)标准(3年存留率>90%)。0~6个月两组充填体的磨耗速率最快,随后磨耗速率的下降趋于平缓,BF组4年总磨耗深度为(58±22) μm,Z350组为(54±16) μm(P>0.05), 耐磨性均符合ADA标准(3年磨耗深度<100 μm)。两组充填体均表现为围绕咬合接触区形成凹坑状磨耗(Ⅰ型)和充填体发生均匀磨耗(Ⅱ型)。术后4年,Ⅰ型磨耗充填体中,BF组的磨耗深度大于Z350组(P<0.05),Ⅱ型磨耗充填体中,两组间差异无统计学意义(P>0.05)。结论: 玻璃体的4年存留率和耐磨性均符合ADA标准,用于后牙牙合面重咬合接触区时,玻璃体的耐磨性略逊于复合树脂,用于非重咬合接触区时,二者间无明显差异。
中图分类号:
- R783.1
| [1] | Gordan VV, Blaser PK, Watson RE, et al. A clinical evaluation of a giomer restorative system containing surface prereacted glass ionomer filler: results from a 13-year recall examination[J]. J Am Dent Assoc, 2014,145(10):1036-1043. |
| [2] |
Manhart J, Chen HY, Hickel R. Clinical evaluation of the poste-rior composite Quixfil in class Ⅰ and Ⅱ cavities: 4-year follow-up of a randomized controlled trial[J]. J Adhes Dent, 2010,12(3):237-243.
doi: 10.3290/j.jad.a17551 pmid: 20157663 |
| [3] |
Oz FD, Ergin E, Canatan S. Twenty-four-month clinical perfor-mance of different universal adhesives in etch-and-rinse, selective etching and self-etch application modes in NCCL: a randomized controlled clinical trial[J]. J Appl Oral Sci, 2019,27:e20180358.
doi: 10.1590/1678-7757-2018-0358 pmid: 30994773 |
| [4] |
Koc Vural U, Meral E, Ergin E, et al. Twenty-four-month clinical performance of a glass hybrid restorative in non-carious cervical lesions of patients with bruxism: a split-mouth, randomized clinical trial[J]. Clin Oral Investig, 2020,24(3):1229-1238.
doi: 10.1007/s00784-019-02986-x pmid: 31297658 |
| [5] |
Hayashi M, Wilson NH. Failure risk of posterior composites with post-operative sensitivity[J]. Oper Dent, 2003,28(6):681-688.
pmid: 14653280 |
| [6] |
Heintze SD. Clinical relevance of tests on bond strength, microleakage and marginal adaptation[J]. Dent Mater, 2013,29(1):59-84.
doi: 10.1016/j.dental.2012.07.158 |
| [7] |
Naoum S, Ellakwa A, Martin F, et al. Fluoride release, recharge and mechanical property stability of various fluoride-containing resin composites[J]. Oper Dent, 2011,36(4):422-432.
doi: 10.2341/10-414-L pmid: 21819201 |
| [8] |
Ikemura K, Tay FR, Endo T, et al. A review of chemical-approach and ultramorphological studies on the development of fluoride-releasing dental adhesives comprising new pre-reacted glass ionomer (PRG) fillers[J]. Dent Mater J, 2008,27(3):315-339.
doi: 10.4012/dmj.27.315 pmid: 18717159 |
| [9] |
Saku S, Kotake H, Scougall-Vilchis RJ, et al. Antibacterial acti-vity of composite resin with glass-ionomer filler particles[J]. Dent Mater J, 2010,29(2):193-198.
doi: 10.4012/dmj.2009-050 pmid: 20379030 |
| [10] |
Kitagawa H, Miki-Oka S, Mayanagi G, et al. Inhibitory effect of resin composite containing S-PRG filler on Streptococcus mutans glucose metabolism[J]. J Dent, 2018,70:92-96.
doi: 10.1016/j.jdent.2017.12.017 pmid: 29294301 |
| [11] |
Kakuta K, Wonglamsam A, Goto S, et al. Surface textures of composite resins after combined wear test simulating both occlusal wear and brushing wear[J]. Dent Mater J, 2012,31(1):61-67.
doi: 10.4012/dmj.2010-091 |
| [12] |
Ruivo MA, Pacheco RR, Sebold M, et al. Surface roughness and filler particles characterization of resin-based composites[J]. Microsc Res Tech, 2019,82(10):1756-1767.
doi: 10.1002/jemt.23342 pmid: 31313442 |
| [13] |
Condo R, Cerroni L, Pasquantonio G, et al. A deep morphological characterization and comparison of different dental restorative materials[J]. Biomed Res Int, 2017,2017:7346317.
doi: 10.1155/2017/7346317 pmid: 28752095 |
| [14] |
Heintze SD, Faouzi M, Rousson V, et al. Correlation of wear in vivo and six laboratory wear methods[J]. Dent Mater, 2012,28(9):961-973.
doi: 10.1016/j.dental.2012.04.006 |
| [15] |
Heintze SD, Ilie N, Hickel R, et al. Laboratory mechanical parameters of composite resins and their relation to fractures and wear in clinical trials: A systematic review[J]. Dent Mater, 2017,33(3):e101-e114.
doi: 10.1016/j.dental.2016.11.013 pmid: 27993372 |
| [16] |
Hickel R, Roulet JF, Bayne S, et al. Recommendations for conducting controlled clinical studies of dental restorative materials[J]. Clin Oral Investig, 2007,11(1):5-33.
doi: 10.1007/s00784-006-0095-7 pmid: 17262225 |
| [17] |
Leinfelder KF, Taylor DF, Barkmeier WW, et al. Quantitative wear measurement of posterior composite resins[J]. Dent Mater, 1986,2(5):198-201.
doi: 10.1016/S0109-5641(86)80013-6 pmid: 3468024 |
| [18] |
Mehl A, Gloger W, Kunzelmann KH, et al. A new optical 3-D device for the detection of wear[J]. J Dent Res, 1997,76(11):1799-1807.
doi: 10.1177/00220345970760111201 pmid: 9372798 |
| [19] |
Palotie U, Eronen AK, Vehkalahti K, et al. Longevity of 2- and 3-surface restorations in posterior teeth of 25- to 30-year-old attending Public Dental Service: A 13-year observation[J]. J Dent, 2017,62:13-17.
doi: 10.1016/j.jdent.2017.05.012 pmid: 28529175 |
| [20] | The American Dental Association. ADA acceptance program guidelines: resin based composites for posterior restorations [R]. Chicago: ADA Council on Scientific Affairs, 2001. |
| [21] |
Lempel E, Toth A, Fabian T, et al. Retrospective evaluation of posterior direct composite restorations: 10-year findings[J]. Dent Mater, 2015,31(2):115-122.
doi: 10.1016/j.dental.2014.11.001 pmid: 25480695 |
| [22] |
Demarco FF, Correa MB, Cenci MS, et al. Longevity of posterior composite restorations: not only a matter of materials[J]. Dent Mater, 2012,28(1):87-101.
doi: 10.1016/j.dental.2011.09.003 |
| [23] |
Hewlett ER, Orro ME, Clark GT. Accuracy testing of three-dimensional digitizing systems[J]. Dent Mater, 1992,8(1):49-53.
doi: 10.1016/0109-5641(92)90053-f pmid: 1521684 |
| [24] |
Thongthammachat S, Moore BK, Barco MT 2nd, et al. Dimensional accuracy of dental casts: influence of tray material, impression material, and time[J]. J Prosthodont, 2002,11(2):98-108.
pmid: 12087547 |
| [25] |
Palaniappan S, Bharadwaj D, Mattar DL, et al. Three-year randomized clinical trial to evaluate the clinical performance and wear of a nanocomposite versus a hybrid composite[J]. Dent Mater, 2009,25(11):1302-1314.
doi: 10.1016/j.dental.2009.06.001 |
| [26] |
Palaniappan S, Elsen L, Lijnen I, et al. Nanohybrid and microfilled hybrid versus conventional hybrid composite restorations: 5-year clinical wear performance[J]. Clin Oral Investig, 2012,16(1):181-190.
doi: 10.1007/s00784-010-0500-0 pmid: 21221678 |
| [27] |
Goldberg AJ, Rydinge E, Santucci EA, et al. Clinical evaluation methods for posterior composite restorations[J]. J Dent Res, 1984,63(12):1387-1391.
doi: 10.1177/00220345840630120901 pmid: 6239885 |
| [28] |
da Rosa Rodolpho PA, Cenci MS, Donassollo TA, et al. A clinical evaluation of posterior composite restorations: 17-year findings[J]. J Dent, 2006,34(7):427-435.
doi: 10.1016/j.jdent.2005.09.006 pmid: 16314023 |
| [29] |
Wilson NHF, Norman RD. Five-year findings of a multiclinical trial for posterior composite[J]. J Dent, 1991,19(3):153-159.
doi: 10.1016/0300-5712(91)90005-j pmid: 1939815 |
| [30] |
Satou N, Khan AM, Satou K, et al. In-vitro and in-vivo wear profile of composite resins[J]. J Oral Rehabil, 1992,19(1):31-37.
doi: 10.1111/j.1365-2842.1992.tb01588.x pmid: 1316435 |
| [31] |
Salgado VE, Cavalcante LM, Silikas N, et al. The influence of nanoscale inorganic content over optical and surface properties of model composites[J]. J Dent, 2013,41(Suppl 5):e45-53.
doi: 10.1016/j.jdent.2013.05.011 |
| [32] |
Lim BS, Ferracane JL, Condon JR, et al. Effect of filler fraction and filler surface treatment on wear of microfilled composites[J]. Dent Mater, 2002,18(1):1-11.
doi: 10.1016/S0109-5641(00)00103-2 |
| [33] |
Garoushi S, Vallittu PK, Lassila L. Characterization of fluoride releasing restorative dental materials[J]. Dent Mater J, 2018,37(2):293-300.
doi: 10.4012/dmj.2017-161 pmid: 29279547 |
| [34] |
Gonulol N, Ozer S, Sen Tunc E. Water sorption, solubility, and color stability of giomer restoratives[J]. J Esthet Restor Dent, 2015,27(5):300-306.
doi: 10.1111/jerd.12119 pmid: 25145876 |
| [35] |
Park CA, Hyun SH, Lee JH, et al. Evaluation of polymerization in fluoride-containing composite resins[J]. J Mater Sci Mater Med, 2007,18(8):1549-1556.
doi: 10.1007/s10856-007-3023-8 pmid: 17437069 |
| [1] | 温奥楠, 张晓会, 杨咏涛, 高梓翔, 李文博, 单珅瑶, 商相宜, 田淯文, 郭殊玮, 王艺蓁, 王勇, 赵一姣. 基于非刚性配准构建三维颜面微笑仿真序列数据的方法[J]. 北京大学学报(医学版), 2026, 58(1): 139-144. |
| [2] | 邵梁, 马雯洁, 陈莹, 丁茜, 张磊. 上颌切牙前伸和正中咬合接触解剖特征的数字化测量与分析[J]. 北京大学学报(医学版), 2026, 58(1): 99-106. |
| [3] | 王翠萍, 陈哲, 程永静. 超微血流成像评估与膝骨关节炎临床症状的关联研究[J]. 北京大学学报(医学版), 2025, 57(6): 1096-1100. |
| [4] | 宋凤岐, 徐心雨, 刘筱菁, 李自力. 上颌骨前部和整体顺时针旋转改善骨性Ⅲ类牙颌面畸形患者鼻旁凹陷的对比[J]. 北京大学学报(医学版), 2025, 57(5): 980-988. |
| [5] | 肖宇嘉, 毛渤淳, 周彦恒. 姿势性微笑的三维形态学研究[J]. 北京大学学报(医学版), 2025, 57(5): 989-995. |
| [6] | 王泽远, 于栓宝, 郑浩轲, 陶金, 范雅峰, 张雪培. 基于临床特征和多参数MRI的前列腺癌盆腔淋巴结转移的术前预测模型[J]. 北京大学学报(医学版), 2025, 57(4): 684-691. |
| [7] | 宁圆, 张晓盈, 李雪, 李原, 何菁, 金月波. 干燥综合征并发乳腺淋巴瘤1例[J]. 北京大学学报(医学版), 2025, 57(4): 808-811. |
| [8] | 孙建军, 马千权, 尹晓亮, 杨辰龙, 张嘉, 陈素华, 吴超, 谢京城, 韩芸峰, 林国中, 司雨, 杨军, 邬海博, 赵强. 任意维度重建磁共振对骶管囊肿进行精准分型对于指导微创手术和康复的意义[J]. 北京大学学报(医学版), 2025, 57(2): 303-308. |
| [9] | 仇师禹, 练洋, 康一帆, 张雷, 蔡义望, 单小峰, 蔡志刚. 基于下颌骨数据库和全连接神经网络的三维检索模型辅助下的下颌骨个性化重建[J]. 北京大学学报(医学版), 2025, 57(2): 360-368. |
| [10] | 马丽娟, 腾雍辉, 王勇, 赵一姣, 张馨月, 秦庆钊, 尹东. 乳牙缺失数字化丝圈间隙保持器的三维有限元分析[J]. 北京大学学报(医学版), 2025, 57(2): 376-383. |
| [11] | 朱玉佳, 沈华, 温奥楠, 高梓翔, 秦庆钊, 单珅瑶, 李文博, 傅湘玲, 赵一姣, 王勇. 三维颌面对称参考平面智能构建的深度学习算法[J]. 北京大学学报(医学版), 2025, 57(1): 113-120. |
| [12] | 徐昕恺, 赵建江, 田素坤, 刘中宁, 赵晓一, 赵晓波, 江腾飞, 陈晓军, 马超, 孙玉春. 集成压缩气流系统扫描头辅助获取液体干扰表面三维数据精度评价[J]. 北京大学学报(医学版), 2025, 57(1): 121-127. |
| [13] | 吴灵, 方嘉琨, 刘筱菁, 李自力, 李阳, 王晓霞. 基于牙颌面畸形患者三维颅面特征相似性度量模型的建立及评估[J]. 北京大学学报(医学版), 2025, 57(1): 128-135. |
| [14] | 蔡文心, 杨琼英, 韩丹, 陈哲, 程永静. 红外热成像检查在风湿病中的应用及展望[J]. 北京大学学报(医学版), 2024, 56(6): 1132-1136. |
| [15] | 邢念增,王明帅,杨飞亚,尹路,韩苏军. 前列腺免活检创新理念的临床实践及其应用前景[J]. 北京大学学报(医学版), 2024, 56(4): 565-566. |
|
||